中国全科医学 ›› 2023, Vol. 26 ›› Issue (03): 348-355.DOI: 10.12114/j.issn.1007-9572.2022.0480
所属专题: 新型冠状病毒肺炎最新文章合辑; 神经系统疾病最新文章合辑; COVID-19疫情防控研究; 脑健康最新研究合辑
皇甫晓娟1,2, 李小娟2,3, 陈敏2,4, 刘吉红2,3, 翟蕊2,3, 蔡志鹏1,2, 李俐涛2,*( )
)
收稿日期:2022-03-31
修回日期:2022-09-20
出版日期:2023-01-20
发布日期:2022-10-27
通讯作者:
李俐涛
基金资助:
HUANGFU Xiaojuan1,2, LI Xiaojuan2,3, CHEN Min2,4, LIU Jihong2,3, ZHAI Rui2,3, CAI Zhipeng1,2, LI Litao2,*( )
)
Received:2022-03-31
Revised:2022-09-20
Published:2023-01-20
Online:2022-10-27
Contact:
LI Litao
About author:摘要: 背景 新型冠状病毒感染(COVID-19)在全球范围蔓延,严重影响人类健康和生活。有研究报道COVID-19可导致血栓性疾病,而脑卒中与血栓事件密切相关。 目的 评估COVID-19对脑卒中患者病死率的影响,并对其可能机制进行探讨,从而为合并COVID-19的脑卒中患者的科学防治提供可靠的临床理论依据。 方法 计算机检索PubMed、EmBase、Web of Science、Cochrane Library、中国知网及万方数据知识服务平台等数据库,收集关于COVID-19对脑卒中患者病死率影响的队列研究或病例对照研究,检索时间为2019年12月至2022年1月。2名研究人员独立进行文献筛选、资料提取,采用纽卡斯尔-渥太华量表(NOS)对文献质量进行评估。采用Meta分析评价COVID-19对脑卒中患者病死率的影响,采用漏斗图评价文献发表偏倚。 结果 共纳入18篇文献,12篇文献质量为高质量,6篇文献质量为中等质量。Meta分析结果显示,合并COVID-19的脑卒中患者病死率、凝血酶原时间(PT)、D-二聚体水平、美国国立卫生研究院卒中量表(NIHSS)评分高于未合并COVID-19的脑卒中患者〔RR=4.16,95%CI(2.82,6.13),P<0.000 01;MD=0.78,95%CI(0.35,1.20),P=0.000 3;MD=1.34,95%CI(0.83,1.84),P<0.000 01;MD=6.66,95%CI(4.54,8.79),P<0.000 01〕,年龄低于未合并COVID-19的脑卒中患者〔MD=-2.04,95%CI(-3.48,-0.61),P=0.005〕。合并COVID-19的脑卒中患者和未合并COVID-19的脑卒中患者活化部分凝血活酶时间(APTT)比较,差异无统计学意义〔MD=2.51,95%CI(-2.69,7.71),P=0.34〕。对合并COVID-19脑卒中患者的病死率绘制漏斗图,结果显示两侧基本对称分布。 结论 COVID-19可增加脑卒中患者病死率,PT、D-二聚体等凝血系统指标的改变可能在其中发挥重要的作用,其预后与年龄、入院时NIHSS评分等相关。
| 第一作者 | 发表年份(年) | 平均年龄(岁) | 样本量(例) | 住院死亡人数(例) | 研究类型 | 结局指标 | |||
|---|---|---|---|---|---|---|---|---|---|
| 病例组 | 对照组 | 病例组 | 对照组 | 病例组 | 对照组 | ||||
| DHAMOON[ | 2021 | 65.9±14.3 | 66.7±15.5 | 105 | 172 | 35 | 22 | 队列研究 | ①②③④⑤⑥ |
| QURESHI[ | 2021 | 68.8±15.1 | 71±14.9 | 8 163 | 199 | — | — | 队列研究 | ①⑥ |
| KATZ[ | 2020 | — | — | 86 | 499 | 25 | 45 | 队列研究 | ① |
| BHATIA[ | 2021 | 58.25±15.19 | 60.59±14.71 | 52 | 355 | 22 | 27 | 病例对照研究 | ①⑥ |
| MEHRPOUR[ | 2020 | 75.60±9.54 | 60.86±18.45 | 10 | 21 | 3 | 2 | 病例对照研究 | ①④⑥ |
| PABLO[ | 2020 | 70.2±8.4 | 70.1±15.3 | 19 | 81 | 5 | 5 | 病例对照 | ①⑥ |
| MATHEW[ | 2021 | 55.66±13.20 | 57.21±11.97 | 60 | 104 | 13 | 0 | 病例对照研究 | ①⑤⑥ |
| MARTÍ-FÀBREGAS[ | 2021 | 71.6±12.3 | 72.4±13.5 | 91 | 610 | 38 | 98 | 队列研究 | ①④⑥ |
| BEKELIS[ | 2020 | — | — | 2 513 | 22 295 | — | — | 队列研究 | ① |
| LIN[ | 2020 | 58.2±18.3 | 65.9±13.9 | 9 | 51 | 4 | 4 | 病例对照研究 | ①②③⑤⑥ |
| TOPCUOGLU[ | 2021 | — | — | 37 | 355 | 18 | 22 | 病例对照研究 | ①③④⑤ |
| PERRY[ | 2020 | — | — | 23 | 177 | — | — | 病例对照研究 | ④ |
| JOHN[ | 2020 | 48.1±10.8 | 58.7 ±14.5 | 19 | 220 | 1 | 4 | 病例对照研究 | ①③⑤⑥ |
| WANG[ | 2021 | — | — | 124 | 226 | 34 | 5 | 队列研究 | ① |
| CIOLLI[ | 2021 | — | — | 26 | 111 | 7 | 10 | 病例对照研究 | ① |
| GARCÍA-LAMBERECHTS[ | 2021 | — | — | 74 814 | 1 388 879 | — | — | 队列研究 | ①②④ |
| KVERNLAND[ | 2020 | — | — | 32 | 46 | 14 | 4 | 队列研究 | ① |
| BENUSSI[ | 2020 | — | — | 43 | 68 | 15 | 4 | 队列研究 | ② |
表1 纳入研究的基本特征
Table 1 Basic characteristics of included studies
| 第一作者 | 发表年份(年) | 平均年龄(岁) | 样本量(例) | 住院死亡人数(例) | 研究类型 | 结局指标 | |||
|---|---|---|---|---|---|---|---|---|---|
| 病例组 | 对照组 | 病例组 | 对照组 | 病例组 | 对照组 | ||||
| DHAMOON[ | 2021 | 65.9±14.3 | 66.7±15.5 | 105 | 172 | 35 | 22 | 队列研究 | ①②③④⑤⑥ |
| QURESHI[ | 2021 | 68.8±15.1 | 71±14.9 | 8 163 | 199 | — | — | 队列研究 | ①⑥ |
| KATZ[ | 2020 | — | — | 86 | 499 | 25 | 45 | 队列研究 | ① |
| BHATIA[ | 2021 | 58.25±15.19 | 60.59±14.71 | 52 | 355 | 22 | 27 | 病例对照研究 | ①⑥ |
| MEHRPOUR[ | 2020 | 75.60±9.54 | 60.86±18.45 | 10 | 21 | 3 | 2 | 病例对照研究 | ①④⑥ |
| PABLO[ | 2020 | 70.2±8.4 | 70.1±15.3 | 19 | 81 | 5 | 5 | 病例对照 | ①⑥ |
| MATHEW[ | 2021 | 55.66±13.20 | 57.21±11.97 | 60 | 104 | 13 | 0 | 病例对照研究 | ①⑤⑥ |
| MARTÍ-FÀBREGAS[ | 2021 | 71.6±12.3 | 72.4±13.5 | 91 | 610 | 38 | 98 | 队列研究 | ①④⑥ |
| BEKELIS[ | 2020 | — | — | 2 513 | 22 295 | — | — | 队列研究 | ① |
| LIN[ | 2020 | 58.2±18.3 | 65.9±13.9 | 9 | 51 | 4 | 4 | 病例对照研究 | ①②③⑤⑥ |
| TOPCUOGLU[ | 2021 | — | — | 37 | 355 | 18 | 22 | 病例对照研究 | ①③④⑤ |
| PERRY[ | 2020 | — | — | 23 | 177 | — | — | 病例对照研究 | ④ |
| JOHN[ | 2020 | 48.1±10.8 | 58.7 ±14.5 | 19 | 220 | 1 | 4 | 病例对照研究 | ①③⑤⑥ |
| WANG[ | 2021 | — | — | 124 | 226 | 34 | 5 | 队列研究 | ① |
| CIOLLI[ | 2021 | — | — | 26 | 111 | 7 | 10 | 病例对照研究 | ① |
| GARCÍA-LAMBERECHTS[ | 2021 | — | — | 74 814 | 1 388 879 | — | — | 队列研究 | ①②④ |
| KVERNLAND[ | 2020 | — | — | 32 | 46 | 14 | 4 | 队列研究 | ① |
| BENUSSI[ | 2020 | — | — | 43 | 68 | 15 | 4 | 队列研究 | ② |
| 第一作者 | 研究人群的选择 | 组间可比性 | 暴露因素测量 | 总分 |
|---|---|---|---|---|
| DHAMOON[ | 3 | 2 | 3 | 8 |
| QURESHI[ | 4 | 1 | 1 | 6 |
| KATZ[ | 4 | 1 | 0 | 5 |
| MARTÍ-FÀBREGAS[ | 4 | 0 | 3 | 7 |
| BEKELIS[ | 4 | 0 | 2 | 6 |
| WANG[ | 4 | 0 | 2 | 6 |
| GARCÍA-LAMBERECHTS[ | 4 | 2 | 3 | 9 |
| KVERNLAND[ | 4 | 1 | 1 | 6 |
| BENUSSI[ | 4 | 2 | 2 | 8 |
表2 纳入队列研究的NOS评分情况(分)
Table 2 Quality of cohort studies assessed using the Newcastle-Ottawa Scale
| 第一作者 | 研究人群的选择 | 组间可比性 | 暴露因素测量 | 总分 |
|---|---|---|---|---|
| DHAMOON[ | 3 | 2 | 3 | 8 |
| QURESHI[ | 4 | 1 | 1 | 6 |
| KATZ[ | 4 | 1 | 0 | 5 |
| MARTÍ-FÀBREGAS[ | 4 | 0 | 3 | 7 |
| BEKELIS[ | 4 | 0 | 2 | 6 |
| WANG[ | 4 | 0 | 2 | 6 |
| GARCÍA-LAMBERECHTS[ | 4 | 2 | 3 | 9 |
| KVERNLAND[ | 4 | 1 | 1 | 6 |
| BENUSSI[ | 4 | 2 | 2 | 8 |
| 第一作者 | 研究人群的选择 | 组间可比性 | 暴露因素测量 | 总分 |
|---|---|---|---|---|
| BHATIA[ | 4 | 1 | 1 | 6 |
| MEHRPOUR[ | 4 | 1 | 2 | 7 |
| PABLO[ | 4 | 1 | 2 | 7 |
| MATHEW[ | 4 | 2 | 2 | 8 |
| LIN[ | 4 | 1 | 3 | 8 |
| TOPCUOGLU[ | 3 | 2 | 2 | 7 |
| PERRY[ | 3 | 2 | 2 | 7 |
| JOHN[ | 4 | 2 | 3 | 9 |
| CIOLLI[ | 4 | 2 | 2 | 8 |
表3 纳入病例对照研究的NOS评分情况(分)
Table 3 Quality of case-control studies assessed using the Newcastle-Ottawa Scale
| 第一作者 | 研究人群的选择 | 组间可比性 | 暴露因素测量 | 总分 |
|---|---|---|---|---|
| BHATIA[ | 4 | 1 | 1 | 6 |
| MEHRPOUR[ | 4 | 1 | 2 | 7 |
| PABLO[ | 4 | 1 | 2 | 7 |
| MATHEW[ | 4 | 2 | 2 | 8 |
| LIN[ | 4 | 1 | 3 | 8 |
| TOPCUOGLU[ | 3 | 2 | 2 | 7 |
| PERRY[ | 3 | 2 | 2 | 7 |
| JOHN[ | 4 | 2 | 3 | 9 |
| CIOLLI[ | 4 | 2 | 2 | 8 |
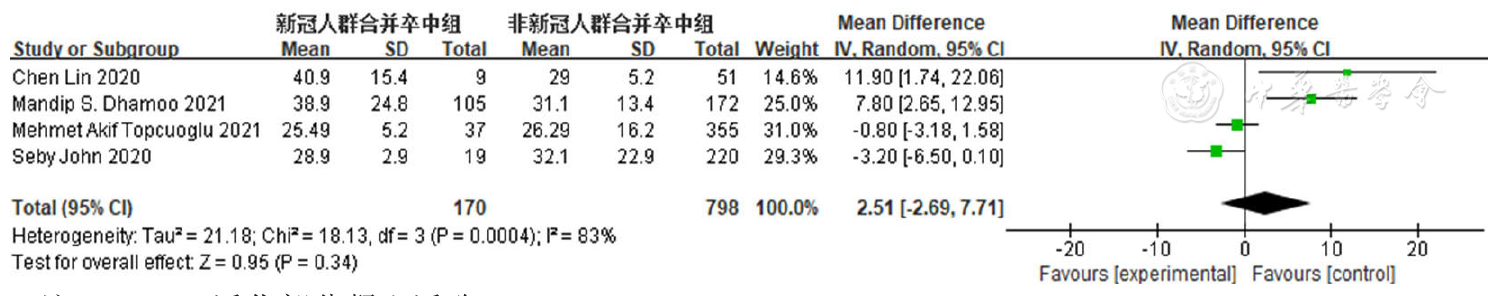
图4 合并COVID-19的脑卒中患者和未合并COVID-19的脑卒中患者APTT比较的森林图注:APTT=活化部分凝血活酶
Figure 4 Forest plot comparing activated partial thromboplastin time in stroke patients with and without COVID-19
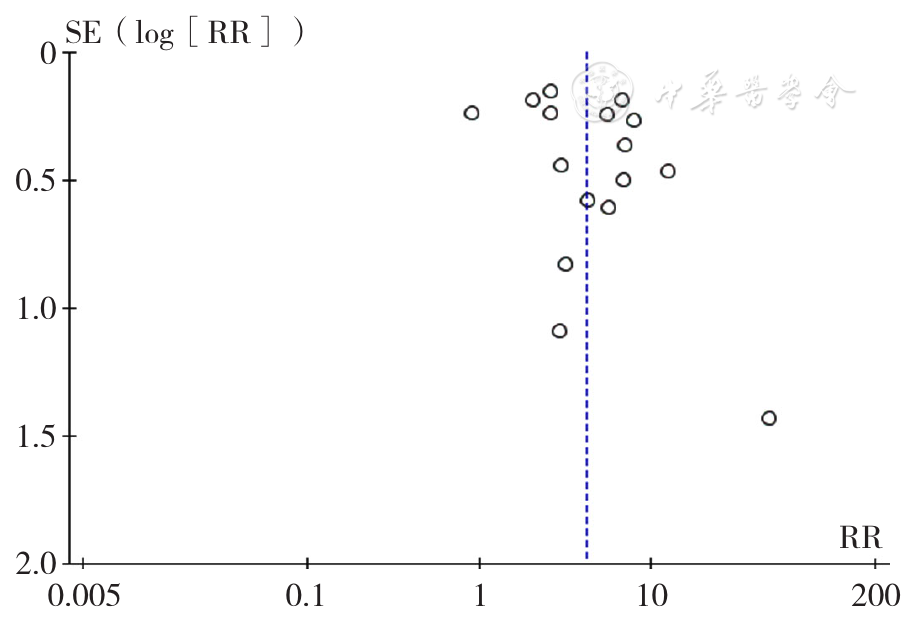
图8 COVID-19对脑卒中患者病死率影响的漏斗图
Figure 8 Funnel plot assessing the potential publication bias in included studies on the impact of COVID-19 on stroke mortality
| [1] |
|
| [2] |
|
| [3] |
|
| [4] |
|
| [5] |
|
| [6] |
|
| [7] |
|
| [8] |
|
| [9] |
|
| [10] |
|
| [11] |
|
| [12] |
|
| [13] |
|
| [14] |
中华医学会神经病学分会,中华医学会神经病学分会脑血管病学组. 中国急性缺血性脑卒中诊治指南2018[J]. 中华神经科杂志,2018,51(9):666-682. DOI:10.3760/cma.j.issn.1006-7876.2018.09.004.
|
| [15] |
|
| [16] |
|
| [17] |
|
| [18] |
|
| [19] |
|
| [20] |
|
| [21] |
|
| [22] |
|
| [23] |
|
| [24] |
|
| [25] |
|
| [26] |
|
| [27] |
|
| [28] |
|
| [29] |
|
| [30] |
|
| [31] |
|
| [32] |
|
| [33] |
|
| [34] |
|
| [35] |
|
| [36] |
|
| [37] |
|
| [38] |
|
| [39] |
|
| [40] |
|
| [41] |
|
| [42] |
|
| [43] |
|
| [44] |
|
| [45] |
|
| [46] |
|
| [47] |
|
| [48] |
|
| [1] | 田晨, 刘佳宁, 田金徽, 葛龙. 动态系统评价制作方法与流程[J]. 中国全科医学, 2025, 28(30): 3853-3860. |
| [2] | 许佳兰, 阎红, 文君, 周紫彤, 王思宇. 老年癌症患者潜在不适当用药发生率的Meta分析[J]. 中国全科医学, 2025, 28(30): 3815-3822. |
| [3] | 全家霖, 朱琳, 苏煜, 陈泽恺, 陈梓淇, 张卓凡. 运动方式对超重或肥胖儿童青少年执行功能改善效果的网状Meta分析[J]. 中国全科医学, 2025, 28(27): 3422-3431. |
| [4] | 张天宇, 于海搏, 陈飞, 李新, 张佳佳, 詹晓凯, 申曼, 汤然, 范斯斌, 赵凤仪, 黄仲夏. POEMS综合征全身系统性治疗疗效和安全性的Meta分析[J]. 中国全科医学, 2025, 28(27): 3447-3455. |
| [5] | 尚忠华, 蒋芝月, 黄朝晖, 杨星, 刘海燕, 张丽. 1990—2021年中国宫颈癌疾病负担趋势分析及2022—2035年预测研究[J]. 中国全科医学, 2025, 28(26): 3314-3320. |
| [6] | 罗新宇, 刘瑾, 陈海龙. 1990—2021年中国和全球胰腺炎疾病负担趋势分析及2022—2031年预测研究[J]. 中国全科医学, 2025, 28(26): 3321-3327. |
| [7] | 丁香, 刘健, 陈晓露, 张先恒. 中草药降低类风湿关节炎合并链球菌感染患者再入院的风险:一项匹配队列研究[J]. 中国全科医学, 2025, 28(24): 3005-3012. |
| [8] | 蒋世华, 朱政, 任盈盈, 朱垚磊, 王越, 高希彬. 中国儿童青少年近视患病率及影响因素的Meta分析[J]. 中国全科医学, 2025, 28(24): 3043-3052. |
| [9] | 王笑林, 李秋月, 周彦君, 张金辉, 梁涛. 转移性结直肠癌患者呋喹替尼治疗相关心血管毒性发生率和风险的Meta分析[J]. 中国全科医学, 2025, 28(23): 2934-2940. |
| [10] | 周倩, 吴晓敏, 王宝华, 严若菡, 蔚苗, 吴静. 胃癌发生风险的列线图预测模型研究[J]. 中国全科医学, 2025, 28(23): 2870-2877. |
| [11] | 李浩, 李江涛, 刘丹, 王建军. 贝利尤单抗和阿尼鲁单抗及泰它西普治疗系统性红斑狼疮疗效和安全性的网状Meta分析[J]. 中国全科医学, 2025, 28(23): 2924-2933. |
| [12] | 杨继, 张垚, 赵英强, 张秋月. 中医三级防控模式对冠心病与脑卒中患者的管理效能评价:一项单中心前瞻性队列研究[J]. 中国全科医学, 2025, 28(22): 2750-2761. |
| [13] | 胡婉琴, 余深艳, 曹学华, 向凤, 贾钰. 中国儿童性早熟影响因素的Meta分析[J]. 中国全科医学, 2025, 28(21): 2661-2671. |
| [14] | 阿迪力·吐尔孙, 程刚. 非奈利酮治疗2型糖尿病肾病有效性和安全性的Meta分析[J]. 中国全科医学, 2025, 28(21): 2686-2691. |
| [15] | 马盼盼, 王思静, 游娜, 丁大法, 鲁一兵. Danuglipron与Orforglipron治疗2型糖尿病疗效及安全性的Meta分析[J]. 中国全科医学, 2025, 28(21): 2679-2685. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||





