

Chinese General Practice ›› 2023, Vol. 26 ›› Issue (08): 917-926.DOI: 10.12114/j.issn.1007-9572.2022.0592
Special Issue: 心血管最新文章合辑
• Original Research • Previous Articles Next Articles
Received:2022-04-12
Revised:2022-10-10
Published:2023-03-15
Online:2022-11-24
Contact:
HE Sen
通讯作者:
何森
作者简介:基金资助:
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.chinagp.net/EN/10.12114/j.issn.1007-9572.2022.0592
| 变量 | 定义 | 赋值原则 |
|---|---|---|
| 年龄 | 首次评估时的年龄[ | 连续性变量:岁 |
| 既往TE事件 | 根据CHA2DS2-VASc评分模型中的相关定义,为:缺血性脑卒中、短暂性脑缺血发作或外周动脉栓塞[ | 二分类变量:是/否 |
| 血管疾病 | 根据CHA2DS2-VASc评分模型中的相关定义,为:陈旧心肌梗死、外周动脉疾病或主动脉斑块[ | 二分类变量:是/否 |
| 高血压 | 血压值持续或非同日3次以上超过标准血压,即3次非同日收缩压≥140 mm Hg和/或舒张压≥90 mm Hg者,则诊断高血压;如既往诊断高血压,目前服用药物情况下血压处于参考范围,也诊断为高血压[ | 二分类变量:是/否 |
| 糖尿病 | 空腹血糖水平≥7 mmol/L,或有医生诊断的糖尿病史,或服用降糖药物[ | 二分类变量:是/否 |
| 心房颤动 | 诊断依据:存在心房颤动病史,或常规心电图提示心房颤动,或动态心电图提示心房颤动[ | 二分类变量:是/否 |
| MWT | 超声心动图测定的MWT | 连续性变量:mm |
| LA内径 | 超声心动图测定的LA前后径 | 连续性变量:mm |
| LVOTO | 左心室流出道静息压力阶差≥30 mm Hg[ | 二分类变量:是/否 |
| NYHA心功能分级 | Ⅰ级:有心脏病但体力活动不受限制;日常体力活动不引起明显的疲乏、心悸、呼吸困难、心绞痛等症状 | 二分类变量:Ⅲ/Ⅳ级为是,Ⅰ/Ⅱ级为否 |
| Ⅱ级:体力活动轻度受限;休息时无自觉症状,日常活动可出现较明显的上述症状,休息后很快缓解 | ||
| Ⅲ级:体力活动明显受限;休息时可无症状,轻于日常活动即引起上述症状,休息较长时间后方可缓解 | ||
| Ⅳ级:不能从事任何体力活动;休息时亦有心衰的症状,体力活动后明显加重 | ||
| LVEF | 超声心动图测定的左心室射血分数 | 连续性变量:% |
Table 1 Definitions and weight assignment principles of candidate variables
| 变量 | 定义 | 赋值原则 |
|---|---|---|
| 年龄 | 首次评估时的年龄[ | 连续性变量:岁 |
| 既往TE事件 | 根据CHA2DS2-VASc评分模型中的相关定义,为:缺血性脑卒中、短暂性脑缺血发作或外周动脉栓塞[ | 二分类变量:是/否 |
| 血管疾病 | 根据CHA2DS2-VASc评分模型中的相关定义,为:陈旧心肌梗死、外周动脉疾病或主动脉斑块[ | 二分类变量:是/否 |
| 高血压 | 血压值持续或非同日3次以上超过标准血压,即3次非同日收缩压≥140 mm Hg和/或舒张压≥90 mm Hg者,则诊断高血压;如既往诊断高血压,目前服用药物情况下血压处于参考范围,也诊断为高血压[ | 二分类变量:是/否 |
| 糖尿病 | 空腹血糖水平≥7 mmol/L,或有医生诊断的糖尿病史,或服用降糖药物[ | 二分类变量:是/否 |
| 心房颤动 | 诊断依据:存在心房颤动病史,或常规心电图提示心房颤动,或动态心电图提示心房颤动[ | 二分类变量:是/否 |
| MWT | 超声心动图测定的MWT | 连续性变量:mm |
| LA内径 | 超声心动图测定的LA前后径 | 连续性变量:mm |
| LVOTO | 左心室流出道静息压力阶差≥30 mm Hg[ | 二分类变量:是/否 |
| NYHA心功能分级 | Ⅰ级:有心脏病但体力活动不受限制;日常体力活动不引起明显的疲乏、心悸、呼吸困难、心绞痛等症状 | 二分类变量:Ⅲ/Ⅳ级为是,Ⅰ/Ⅱ级为否 |
| Ⅱ级:体力活动轻度受限;休息时无自觉症状,日常活动可出现较明显的上述症状,休息后很快缓解 | ||
| Ⅲ级:体力活动明显受限;休息时可无症状,轻于日常活动即引起上述症状,休息较长时间后方可缓解 | ||
| Ⅳ级:不能从事任何体力活动;休息时亦有心衰的症状,体力活动后明显加重 | ||
| LVEF | 超声心动图测定的左心室射血分数 | 连续性变量:% |
| 变量 | 未发生TE事件(n=471) | 发生TE事件(n=42) | χ2(Z)值 | P值 |
|---|---|---|---|---|
| 性别(男/女) | 267/204 | 16/26 | 4.664 | 0.031 |
| 年龄〔M(P25,P75),岁〕 | 57.0(44.0,66.0) | 66.0(51.3,73.0) | 12.027a | 0.001 |
| 既往TE事件〔n(%)〕 | 20(4.25) | 7(16.67) | — | 0.004 |
| 血管疾病〔n(%)〕 | 35(7.43) | 5(11.90) | — | 0.360 |
| 高血压〔n(%)〕 | 147(31.21) | 15(35.71) | 0.184 | 0.668 |
| 糖尿病〔n(%)〕 | 33(7.01) | 7(16.67) | — | 0.035 |
| 心房颤动〔n(%)〕 | 65(13.80) | 22(52.38) | 38.063 | <0.001 |
| MWT〔M(P25,P75),mm〕 | 19.0(17.0,22.0) | 18.0(16.0,21.0) | 2.466a | 0.116 |
| LA内径〔M(P25,P75),mm〕 | 40.0(35.0,45.0) | 43.0(38.2,46.0) | 6.955a | 0.008 |
| LVOTO〔n(%)〕 | 208(44.16) | 14(33.33) | 1.427 | 0.232 |
| NYHA心功能Ⅲ/Ⅳ级〔n(%)〕 | 163(34.61) | 13(30.95) | 0.095 | 0.758 |
| LVEF〔M(P25,P75),%〕 | 69.0(63.0,73.0) | 67.5(62.2,70.0) | 3.712a | 0.054 |
| 阿司匹林〔n(%)〕 | 84(17.83) | 10(23.81) | 0.564 | 0.453 |
| 氯吡格雷〔n(%)〕 | 28(5.94) | 3(7.14) | — | 0.733 |
| 华法林〔n(%)〕 | 35(7.43) | 10(23.81) | — | 0.002 |
Table 2 Baseline characteristics in hypertrophic cardiomyopathy patients with and without thrombotic events
| 变量 | 未发生TE事件(n=471) | 发生TE事件(n=42) | χ2(Z)值 | P值 |
|---|---|---|---|---|
| 性别(男/女) | 267/204 | 16/26 | 4.664 | 0.031 |
| 年龄〔M(P25,P75),岁〕 | 57.0(44.0,66.0) | 66.0(51.3,73.0) | 12.027a | 0.001 |
| 既往TE事件〔n(%)〕 | 20(4.25) | 7(16.67) | — | 0.004 |
| 血管疾病〔n(%)〕 | 35(7.43) | 5(11.90) | — | 0.360 |
| 高血压〔n(%)〕 | 147(31.21) | 15(35.71) | 0.184 | 0.668 |
| 糖尿病〔n(%)〕 | 33(7.01) | 7(16.67) | — | 0.035 |
| 心房颤动〔n(%)〕 | 65(13.80) | 22(52.38) | 38.063 | <0.001 |
| MWT〔M(P25,P75),mm〕 | 19.0(17.0,22.0) | 18.0(16.0,21.0) | 2.466a | 0.116 |
| LA内径〔M(P25,P75),mm〕 | 40.0(35.0,45.0) | 43.0(38.2,46.0) | 6.955a | 0.008 |
| LVOTO〔n(%)〕 | 208(44.16) | 14(33.33) | 1.427 | 0.232 |
| NYHA心功能Ⅲ/Ⅳ级〔n(%)〕 | 163(34.61) | 13(30.95) | 0.095 | 0.758 |
| LVEF〔M(P25,P75),%〕 | 69.0(63.0,73.0) | 67.5(62.2,70.0) | 3.712a | 0.054 |
| 阿司匹林〔n(%)〕 | 84(17.83) | 10(23.81) | 0.564 | 0.453 |
| 氯吡格雷〔n(%)〕 | 28(5.94) | 3(7.14) | — | 0.733 |
| 华法林〔n(%)〕 | 35(7.43) | 10(23.81) | — | 0.002 |
| 变量 | 单因素Cox回归分析 | 多因素Cox回归分析 | ||||
|---|---|---|---|---|---|---|
| HR(95%CI) | P值 | β | HR(95%CI) | P值 | ||
| 性别(以男性为参照) | ||||||
| 女 | 1.85(0.99,3.45) | 0.053 | — | — | — | |
| 年龄(岁,以<50岁为参照) | ||||||
| 50~<70 | 1.69(0.73,3.92) | 0.221 | 0.329 | 1.39(0.59,3.28) | 0.452 | |
| ≥70 | 4.46(1.92,10.4) | <0.001 | 1.107 | 3.02(1.25,7.34) | 0.014 | |
| 既往TE事件 | 5.62(2.49,12.7) | <0.001 | 1.174 | 3.24(1.38,7.61) | 0.007 | |
| 血管疾病1 | .92(0.75,4.90) | 0.174 | — | — | — | |
| 高血压 | 1.30(0.69,2.44) | 0.420 | — | — | — | |
| 糖尿病 | 2.20(0.97,4.94) | 0.058 | — | — | — | |
| 心房颤动 | 5.95(3.24,10.90) | <0.001 | 1.472 | 4.36(2.31,8.23) | <0.001 | |
| MWT(mm,以<20.0 mm为参照) | ||||||
| 20.0~<25.0 | 0.98(0.51,1.88) | 0.949 | — | — | — | |
| 25.0~<30.0 | 0.49(0.12,2.09) | 0.338 | — | — | — | |
| ≥30.0 | 0(0,Inf) | 0.996 | — | — | — | |
| LA内径(mm,以<35.0 mm为参照) | ||||||
| 35.0~<40.0 | 1.52(0.47,4.95) | 0.484 | — | — | — | |
| 40.0~<45.0 | 3.14(1.03,9.55) | 0.044 | — | — | — | |
| ≥45.0 | 2.80(0.93,8.44) | 0.067 | — | — | — | |
| LVOTO | 0.72(0.38,1.37) | 0.314 | — | — | — | |
| NYHA心功能分级(以Ⅰ/Ⅱ级为参照) | ||||||
| Ⅲ/Ⅳ级 | 1.05(0.54,2.02) | 0.887 | — | — | — | |
| LVEF(%,以<50.0%为参照) | ||||||
| 50.0~<70.0 | 0.56(0.17,1.86) | 0.344 | -0.981 | 0.37(0.11,1.29) | 0.120 | |
| ≥70.0 | 0.31(0.09,1.08) | 0.067 | -1.407 | 0.24(0.07,0.91) | 0.035 | |
| 阿司匹林 | 1.35(0.67,2.76) | 0.402 | — | — | — | |
| 氯吡格雷 | 1.26(0.39,4.07) | 0.702 | — | — | — | |
| 华法林 | 4.33(2.11,8.89) | <0.001 | — | — | — | |
Table 3 Univariate and multvariate Cox regression analyses for factors predicting the risk of thrombotic events in hypertrophic cardiomyopathy patients
| 变量 | 单因素Cox回归分析 | 多因素Cox回归分析 | ||||
|---|---|---|---|---|---|---|
| HR(95%CI) | P值 | β | HR(95%CI) | P值 | ||
| 性别(以男性为参照) | ||||||
| 女 | 1.85(0.99,3.45) | 0.053 | — | — | — | |
| 年龄(岁,以<50岁为参照) | ||||||
| 50~<70 | 1.69(0.73,3.92) | 0.221 | 0.329 | 1.39(0.59,3.28) | 0.452 | |
| ≥70 | 4.46(1.92,10.4) | <0.001 | 1.107 | 3.02(1.25,7.34) | 0.014 | |
| 既往TE事件 | 5.62(2.49,12.7) | <0.001 | 1.174 | 3.24(1.38,7.61) | 0.007 | |
| 血管疾病1 | .92(0.75,4.90) | 0.174 | — | — | — | |
| 高血压 | 1.30(0.69,2.44) | 0.420 | — | — | — | |
| 糖尿病 | 2.20(0.97,4.94) | 0.058 | — | — | — | |
| 心房颤动 | 5.95(3.24,10.90) | <0.001 | 1.472 | 4.36(2.31,8.23) | <0.001 | |
| MWT(mm,以<20.0 mm为参照) | ||||||
| 20.0~<25.0 | 0.98(0.51,1.88) | 0.949 | — | — | — | |
| 25.0~<30.0 | 0.49(0.12,2.09) | 0.338 | — | — | — | |
| ≥30.0 | 0(0,Inf) | 0.996 | — | — | — | |
| LA内径(mm,以<35.0 mm为参照) | ||||||
| 35.0~<40.0 | 1.52(0.47,4.95) | 0.484 | — | — | — | |
| 40.0~<45.0 | 3.14(1.03,9.55) | 0.044 | — | — | — | |
| ≥45.0 | 2.80(0.93,8.44) | 0.067 | — | — | — | |
| LVOTO | 0.72(0.38,1.37) | 0.314 | — | — | — | |
| NYHA心功能分级(以Ⅰ/Ⅱ级为参照) | ||||||
| Ⅲ/Ⅳ级 | 1.05(0.54,2.02) | 0.887 | — | — | — | |
| LVEF(%,以<50.0%为参照) | ||||||
| 50.0~<70.0 | 0.56(0.17,1.86) | 0.344 | -0.981 | 0.37(0.11,1.29) | 0.120 | |
| ≥70.0 | 0.31(0.09,1.08) | 0.067 | -1.407 | 0.24(0.07,0.91) | 0.035 | |
| 阿司匹林 | 1.35(0.67,2.76) | 0.402 | — | — | — | |
| 氯吡格雷 | 1.26(0.39,4.07) | 0.702 | — | — | — | |
| 华法林 | 4.33(2.11,8.89) | <0.001 | — | — | — | |
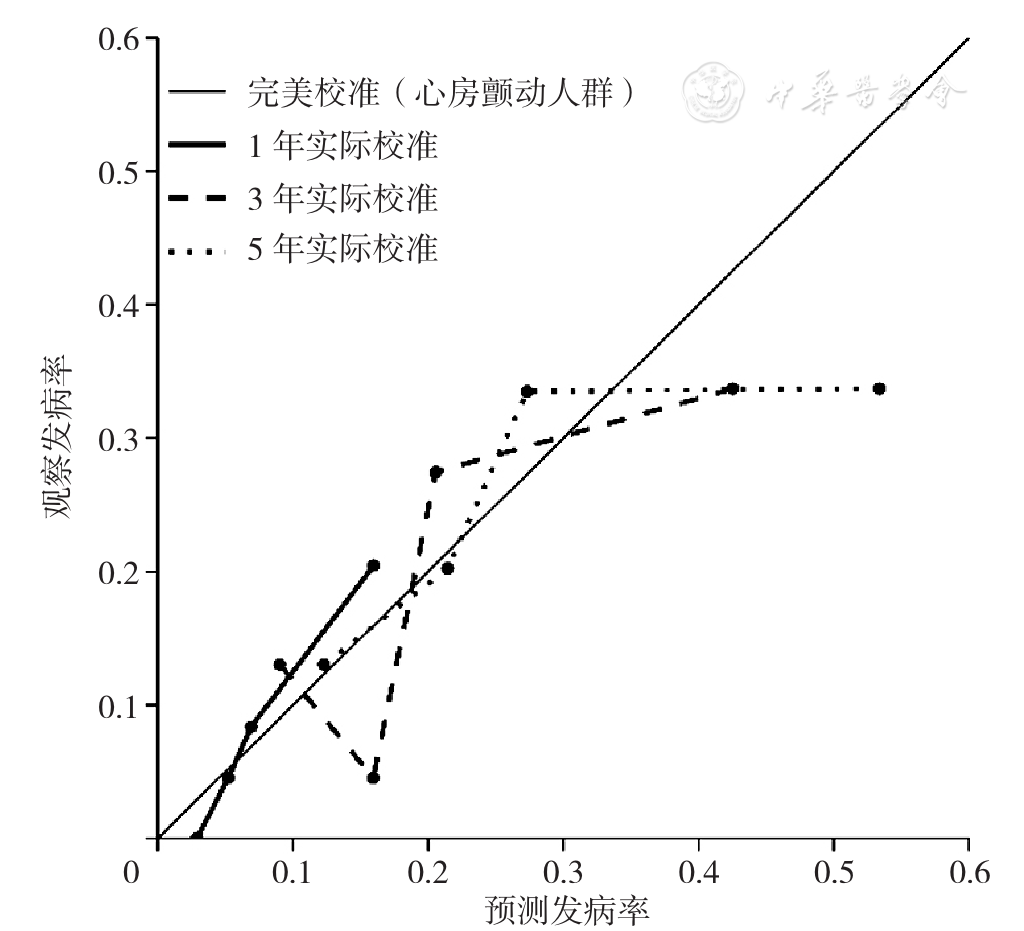
Figure 5 Calibration plots for predicted versus observed 1-,3-,5-year risk of thrombotic events for hypertrophic cardiomyopathy patients with atrial fibrillation
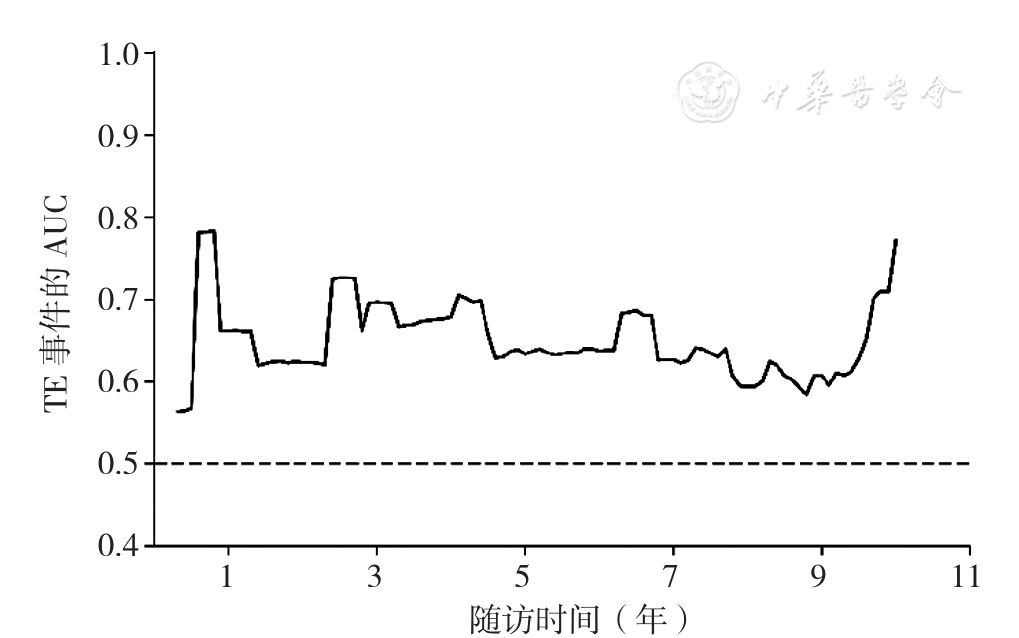
Figure 6 Predictive power of SAAE score for 1-,3- and 5-year risk of thrombotic events for hypertrophic cardiomyopathy patients without atrial fibrillation
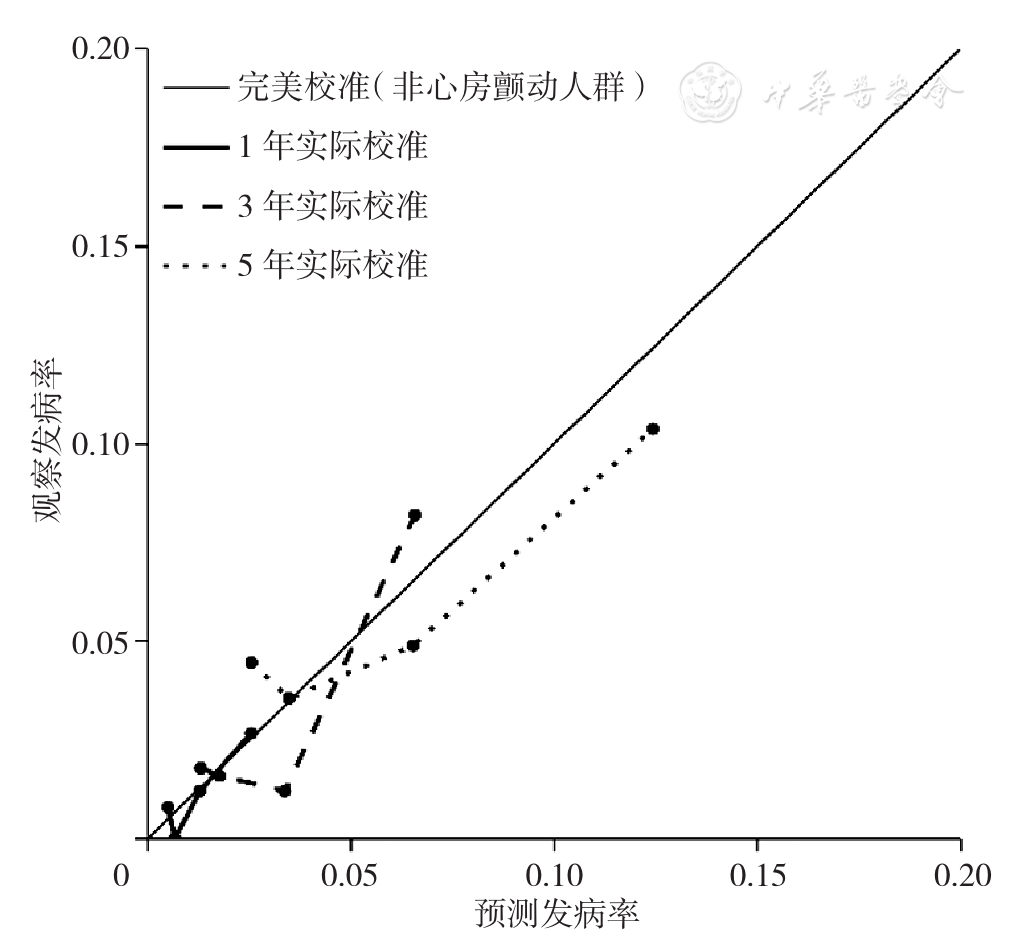
Figure 7 Calibration plots for predicted versus observed 1-,3-,5-year risk of thrombotic events for hypertrophic cardiomyopathy patients without atrial fibrillation
| 分类 | 低风险 | 中风险 | 高风险 |
|---|---|---|---|
| 整体人群 | <7.56 | 7.56~<17.38 | ≥17.38 |
| 心房颤动人群 | <17.56 | 17.56~<21.42 | ≥21.42 |
| 非心房颤动人群 | <3.87 | 3.87~<11.25 | ≥11.25 |
Table 4 Cutoff points of SAAE score for low,moderate and high risk of thrombotic events in different populations
| 分类 | 低风险 | 中风险 | 高风险 |
|---|---|---|---|
| 整体人群 | <7.56 | 7.56~<17.38 | ≥17.38 |
| 心房颤动人群 | <17.56 | 17.56~<21.42 | ≥21.42 |
| 非心房颤动人群 | <3.87 | 3.87~<11.25 | ≥11.25 |
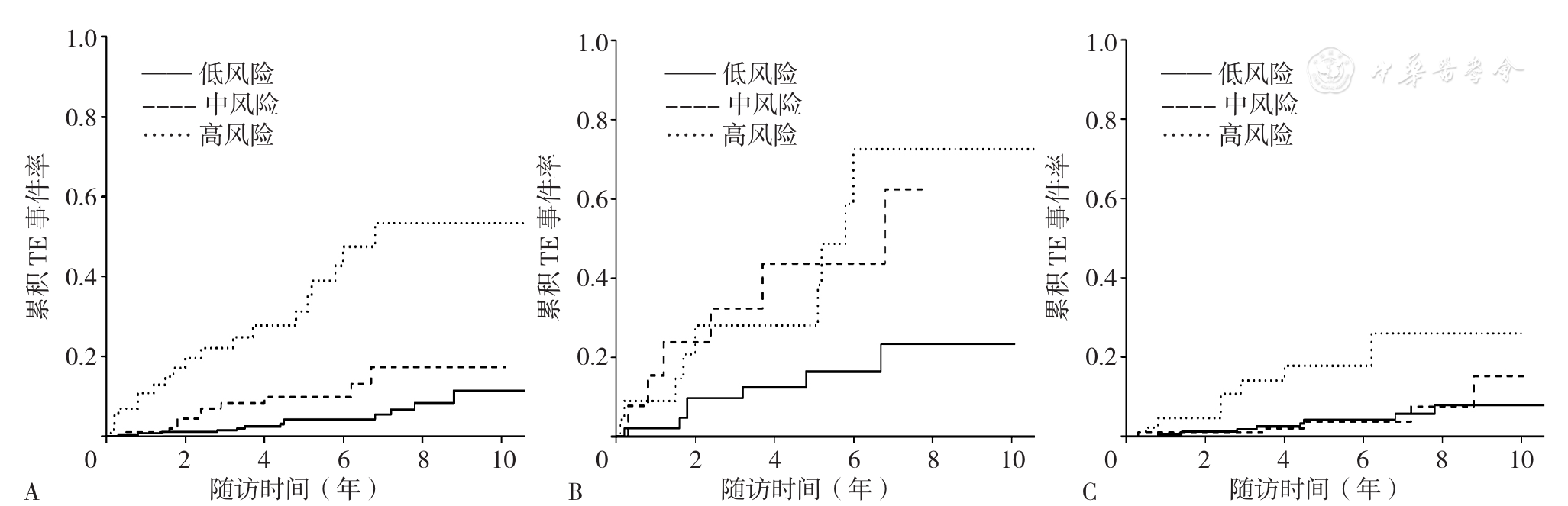
Figure 8 Kaplan-Meier analysis showing cumulative thrombotic events in hypertrophic cardiomyopathy patients with low,moderate or high thrombotic risk predicted by SAAE score
| 人群 | 评分模型 | 整体 | 1年 | 3年 | 5年 | ||||
|---|---|---|---|---|---|---|---|---|---|
| Harrell's C-指数 | P值 | Harrell's C-指数 | P值 | Harrell's C-指数 | P值 | Harrell's C-指数 | P值 | ||
| 整体人群 | SAAE score | 0.757 | 0.013 | 0.790 | 0.413 | 0.799 | 0.137 | 0.735 | 0.117 |
| HCM Risk-CVA | 0.671 | 0.710 | 0.715 | 0.670 | |||||
| 心房颤动人群 | SAAE score | 0.670 | 0.110 | 0.745 | 0.112 | 0.671 | 0.162 | 0.616 | 0.738 |
| HCM Risk-CVA | 0.560 | 0.557 | 0.538 | 0.587 | |||||
| 非心房颤动人群 | SAAE score | 0.624 | 0.549 | 0.661 | 0.828 | 0.697 | 0.899 | 0.634 | 0.644 |
| HCM Risk-CVA | 0.592 | 0.696 | 0.710 | 0.603 | |||||
Table 5 Comparisons between SAAE score and HCM Risk-CVA score for predicting the risk of thrombotic events in hypertrophic cardiomyopathy
| 人群 | 评分模型 | 整体 | 1年 | 3年 | 5年 | ||||
|---|---|---|---|---|---|---|---|---|---|
| Harrell's C-指数 | P值 | Harrell's C-指数 | P值 | Harrell's C-指数 | P值 | Harrell's C-指数 | P值 | ||
| 整体人群 | SAAE score | 0.757 | 0.013 | 0.790 | 0.413 | 0.799 | 0.137 | 0.735 | 0.117 |
| HCM Risk-CVA | 0.671 | 0.710 | 0.715 | 0.670 | |||||
| 心房颤动人群 | SAAE score | 0.670 | 0.110 | 0.745 | 0.112 | 0.671 | 0.162 | 0.616 | 0.738 |
| HCM Risk-CVA | 0.560 | 0.557 | 0.538 | 0.587 | |||||
| 非心房颤动人群 | SAAE score | 0.624 | 0.549 | 0.661 | 0.828 | 0.697 | 0.899 | 0.634 | 0.644 |
| HCM Risk-CVA | 0.592 | 0.696 | 0.710 | 0.603 | |||||
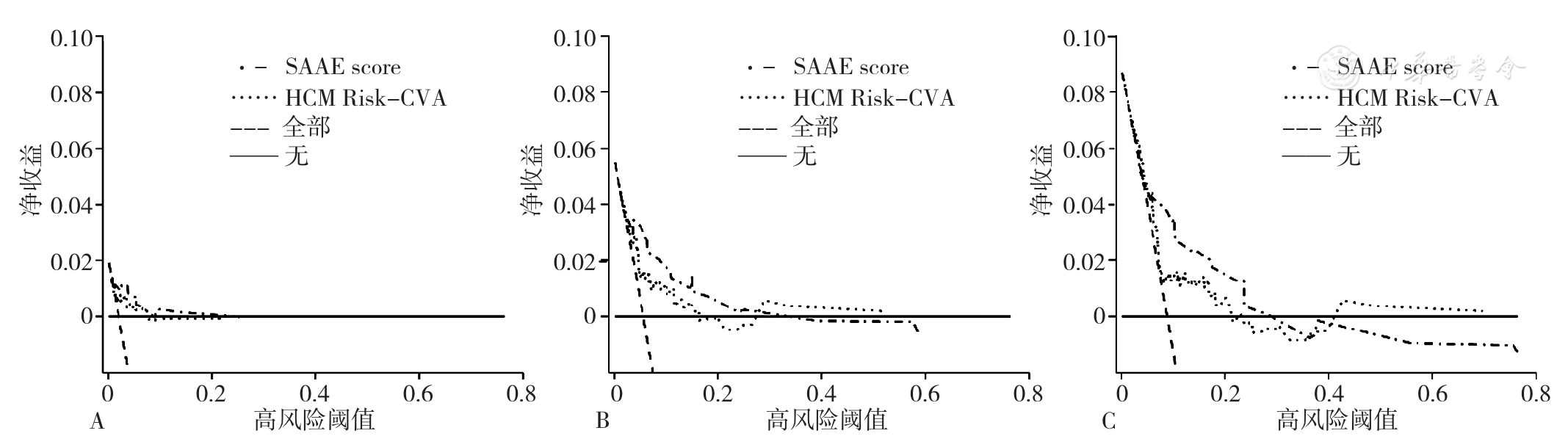
Figure 9 Decision curve analysis of SAAE score and HCM Risk-CVA score for predicting the risk of thrombotic events in hypertrophic cardiomyopathy at different time points
| [1] |
|
| [2] |
|
| [3] |
吴兆苏,姚崇华,赵冬. 我国人群脑卒中发病率、死亡率的流行病学研究[J]. 中华流行病学杂志,2003,24(3):236-239.
|
| [4] |
|
| [5] |
|
| [6] |
|
| [7] |
|
| [8] |
|
| [9] |
|
| [10] |
|
| [11] |
|
| [12] |
|
| [13] |
|
| [14] |
|
| [15] |
|
| [16] |
|
| [17] |
|
| [18] |
|
| [19] |
|
| [20] |
《中国高血压防治指南》修订委员会. 中国高血压防治指南2018年修订版[J]. 心脑血管病防治,2019,19(1):1-44. DOI:10.3969/j.issn.1009-816X.2019.01.001.
|
| [21] |
American Diabetes Association. Standards of medical care in diabetes—2010[J]. Diabetes Care,2010,33(Suppl 1):S11-61. DOI:10.2337/dc10-S011.
|
| [22] |
|
| [23] |
|
| [24] |
|
| [25] |
|
| [26] |
|
| [27] |
顾俊,贾锋鹏,封盼攀. CHADS2与CHA2DS2-VASc评分对非瓣膜病房颤患者左房血栓的风险评估[J]. 南方医科大学学报,2014,34(11):1601-1605.
|
| [28] |
|
| [29] |
|
| [30] |
|
| [31] |
|
| [32] |
|
| [33] |
|
| [34] |
|
| [35] |
|
| [36] |
|
| [37] |
|
| [38] |
|
| [39] |
|
| [40] |
|
| [41] |
|
| [1] | BAI Jiaxin, CHEN Yu, ZHOU Yiheng, LIU Lidi, YANG Rong, YAO Yi, YUAN Bo, ZHANG Yonggang, LEI Yi, ZENG Rui, JIA Yu, LIAO Xiaoyang. Assessment and Treatment of Early-onset Hypertension: Position Statement of the British and Irish Hypertension Association and Its Implications for Clinical Management of Early-onset Hypertension in China [J]. Chinese General Practice, 2025, 28(30): 3741-3746. |
| [2] | XU Jialan, YAN Hong, WEN Jun, ZHOU Zitong, WANG Siyu. Prevalence of Potentially Inappropriate Medication in Older Adults with Cancer: a Meta-analysis [J]. Chinese General Practice, 2025, 28(30): 3815-3822. |
| [3] | ZHANG Peng, LIU Lidi, ZHANG Ying, YANG Ziyu, LIU Changming, TANG Yijun, LIAO Xiaoyang, JIA Yu. Interpretation and Clinical Implications of the 2024 Italian Guidelines for the Management of Adult Individuals with Overweight and Obesity and Metabolic Comorbidities That are Resistant to Behavioral Treatment [J]. Chinese General Practice, 2025, 28(30): 3747-3752. |
| [4] | MA Shuangshuang, XING Yanjiang, ZHANG Jiawei, WANG Jing. Research Progress on Cardiac Energy Metabolic Changes in Heart Failure with Preserved Ejection Fraction [J]. Chinese General Practice, 2025, 28(30): 3831-3840. |
| [5] | LI Ling, LI Yaping, QIAN Shixing, NIE Jing, LU Chunhua, LI Xia. Research on Influencing Factors and Risk Prediction of Cognitive Function in Community-dwelling Middle-aged and Elderly People [J]. Chinese General Practice, 2025, 28(30): 3773-3778. |
| [6] | ZHAO Yuqing, WANG Wei, CHEN Liyuan, YOU Huijuan, WEI Ying, WANG Qinglu, YANG Fengying. Liver Macrophage Polarisation: a New Target for Exercise Prevention and Treatment of Non-alcoholic Fatty Liver Disease [J]. Chinese General Practice, 2025, 28(27): 3456-3465. |
| [7] | ZHANG Hongshi, QU Zihan, SUN Xuefeng, WANG Yufeng, CONG Deyu, ZHANG Ye. Effect of Abdominal Massage on Hypothalamus of Insomnia Rats Based on Proteomics [J]. Chinese General Practice, 2025, 28(27): 3399-3409. |
| [8] | ZHOU Penglong, CHANG Jing, DING Suying, CHEN Jingfeng, WANG Tao, LI Chenyang. Correlation Analysis between Age-Stratified Differences in Fat-to-muscle Ratio and Hyperuricemia [J]. Chinese General Practice, 2025, 28(27): 3375-3384. |
| [9] | WEI Jiaohua, PENG Huiru, PENG Jianye, TAN Wenting, HUANG Jine, FANG Li. Expression of the Serum MOTS-c and Its Correlation with Atrial Remodeling in Patients with Atrial Fibrillation [J]. Chinese General Practice, 2025, 28(26): 3271-3276. |
| [10] | CHEN Junyu, HAN Guangli, LI Chunhong, CHEN Yidi, YANG Nana, LUO Xiaoxi. Classification Study of Self-management Types among Pregnant Women in Rural Areas Based on Cluster Analysis [J]. Chinese General Practice, 2025, 28(26): 3289-3293. |
| [11] | XIANG Xinyue, ZHANG Bingqing, OUYANG Yuqin, TANG Wenjuan, FENG Wenhuan. Impact of Short-term Medical Weight Loss on Atherosclerotic Cardiovascular Disease Risk in Patients with Obesity [J]. Chinese General Practice, 2025, 28(26): 3229-3239. |
| [12] | NIU Ben, ZHU Xiaoqian, YANG Chen, LIANG Wannian, LIU Jue. Evolution and Trends of Domestic and International Research Hotspots in the Field of Large Language Models in Medicine Based on CiteSpace [J]. Chinese General Practice, 2025, 28(25): 3200-3208. |
| [13] | YAN Fanghong, PENG Guotian, ZHANG Guoli, SUN Ruiyi, MA Yuxia, HAN Lin. Matching Analysis of the Content of Chronic Disease Management for the Elderly in Medical Union: Based on the Perspective of "Guidance-Practice-Need" [J]. Chinese General Practice, 2025, 28(25): 3119-3126. |
| [14] | YU Zizi, LIU Duli, LI Ximin, RUAN Chunyi, YIN Xiangyang, CAI Le. Analysis of the Prevalence and Self-management of Hypertension and Its Influencing Factors in Rural [J]. Chinese General Practice, 2025, 28(25): 3137-3143. |
| [15] | LI Jiaxin, LIU Zhonghui, XIE Shuo, FU Zhifang, SUN Dan, JIAO Hongmei. Trajectory in Biomarkers of Metabolic and Inflammatory States as Early Predictors of Chronic Critical Illness in Aging Patients [J]. Chinese General Practice, 2025, 28(24): 2993-2999. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||