中国全科医学 ›› 2026, Vol. 29 ›› Issue (15): 2043-2049.DOI: 10.12114/j.issn.1007-9572.2024.0693
• 论著 • 上一篇
收稿日期:2025-02-20
修回日期:2025-04-22
出版日期:2026-05-20
发布日期:2026-04-14
通讯作者:
郭玮
作者贡献:
蒋丽军、于倩负责研究设计及实施、论文撰写;于倩负责统计学分析;于倩、王伏东负责数据整理;郭玮负责研究设计指导及论文修改。
基金资助:
JIANG Lijun1, YU Qian2, WANG Fudong1, GUO Wei3,*( )
)
Received:2025-02-20
Revised:2025-04-22
Published:2026-05-20
Online:2026-04-14
Contact:
GUO Wei
摘要: 背景 生发基质-脑室内出血(GMH-IVH)是早产儿并发神经系统后遗症的主要原因。早期预测GMH-IVH并进行综合管理,对改善早产儿预后尤为重要。血压波动导致的脑血流(CBF)紊乱以及凝血功能不成熟引起的出血风险增加是GMH-IVH的重要致病因素。 目的 分析血压变异性(BPV)和凝血功能联合检测对胎龄≤32周早产儿GMH-IVH的早期预测价值,并评估其近期预后。 方法 选取2022年6月—2024年6月在扬州大学附属医院新生儿重症监护病房住院并符合标准的胎龄≤32周早产儿106例作为研究对象。按照是否存在GMH-IVH将早产儿分为GMH-IVH组(51例)和非GMH-IVH组(55例);按照短期转归将早产儿分为转归良好组(30例)和转归不良组(21例)。收集入组早产儿的一般资料以及围生期资料,监测各组患儿凝血功能和收缩压(SBP)、舒张压(DBP)的BPV指标,分析各指标与GMH-IVH的关系。采用二元Logistic回归分析探讨早产儿GMH-IVH及转归不良的危险因素,绘制危险因素预测早产儿GMH-IVH及转归不良的ROC曲线,并计算ROC曲线下面积(AUC)。 结果 共纳入106例早产儿,其中男43例(40.6%)、女63例(59.4%)。二元Logistic回归分析结果显示,国际标准化比值(INR)(OR=5.608,95%CI=2.858~8.587,P=0.003)、DBP的标准差(SD)(OR=1.455,95%CI=1.003~2.111,P=0.038)升高是早产儿发生GMH-IVH的独立危险因素;INR、DBP的SD联合预测早产儿发生GMH-IVH的AUC为0.803,其灵敏度为82.4%,特异度为79.7%。二元Logistic回归分析结果显示,INR(OR=3.942,95%CI=1.509~6.680,P=0.025)、DBP的SD(OR=2.334,95%CI=1.013~5.378,P=0.047)升高是早产儿GMH-IVH转归不良的危险因素;INR、DBP的SD联合预测早产儿GMH-IVH转归不良的AUC为0.864,灵敏度为76.2%,特异度为90.0%。 结论 INR、DBP的SD升高是早产儿发生GMH-IVH及其短期预后不良的危险因素,联合INR、DBP的SD监测对于早产儿GMH-IVH的早期识别和预后预测存在一定的临床价值。
中图分类号:
| 指标 | 非GMH-IVH组(n=55) | GMH-IVH组(n=51) | χ2(t)值 | P值 |
|---|---|---|---|---|
| 胎龄( | 29.4±2.0 | 28.5±2.4 | 1.904a | 0.060 |
| 出生体重( | 1 270.0±247.4 | 1 196.0±319.8 | 1.338a | 0.084 |
| 性别[例(%)] | 0.047 | 0.829 | ||
| 男 | 22(40.0) | 21(41.2) | ||
| 女 | 33(60.0) | 30(58.8) | ||
| 阴道分娩[例(%)] | 23(41.8) | 29(56.9) | 2.397 | 0.122 |
| 多胎[例(%)] | 4(7.3) | 8(15.7) | 1.866 | 0.172 |
| 小于胎龄[例(%)] | 8(14.5) | 5(9.8) | 0.553 | 0.457 |
| 5 min Apgar评分≤7分[例(%)] | 7(12.7) | 14(27.5) | 3.611 | 0.057 |
| 孕母高血压[例(%)] | 13(23.6) | 6(11.8) | 2.535 | 0.111 |
| 孕母糖尿病[例(%)] | 5(9.1) | 6(11.8) | 0.203 | 0.652 |
| 有创通气[例(%)] | 5(9.1) | 9(17.6) | 1.690 | 0.194 |
| 产前地塞米松使用[例(%)] | 18(32.7) | 24(47.1) | 2.272 | 0.132 |
| PROM[例(%)] | 9(16.4) | 18(35.3) | 4.995 | 0.025 |
| PDA[例(%)] | 23(41.8) | 30(58.8) | 3.061 | 0.080 |
表1 早产儿一般资料比较
Table 1 Comparison of general data of premature infants
| 指标 | 非GMH-IVH组(n=55) | GMH-IVH组(n=51) | χ2(t)值 | P值 |
|---|---|---|---|---|
| 胎龄( | 29.4±2.0 | 28.5±2.4 | 1.904a | 0.060 |
| 出生体重( | 1 270.0±247.4 | 1 196.0±319.8 | 1.338a | 0.084 |
| 性别[例(%)] | 0.047 | 0.829 | ||
| 男 | 22(40.0) | 21(41.2) | ||
| 女 | 33(60.0) | 30(58.8) | ||
| 阴道分娩[例(%)] | 23(41.8) | 29(56.9) | 2.397 | 0.122 |
| 多胎[例(%)] | 4(7.3) | 8(15.7) | 1.866 | 0.172 |
| 小于胎龄[例(%)] | 8(14.5) | 5(9.8) | 0.553 | 0.457 |
| 5 min Apgar评分≤7分[例(%)] | 7(12.7) | 14(27.5) | 3.611 | 0.057 |
| 孕母高血压[例(%)] | 13(23.6) | 6(11.8) | 2.535 | 0.111 |
| 孕母糖尿病[例(%)] | 5(9.1) | 6(11.8) | 0.203 | 0.652 |
| 有创通气[例(%)] | 5(9.1) | 9(17.6) | 1.690 | 0.194 |
| 产前地塞米松使用[例(%)] | 18(32.7) | 24(47.1) | 2.272 | 0.132 |
| PROM[例(%)] | 9(16.4) | 18(35.3) | 4.995 | 0.025 |
| PDA[例(%)] | 23(41.8) | 30(58.8) | 3.061 | 0.080 |
| 指标 | 非GMH-IVH组(n=55) | GMH-IVH组(n=51) | t(Z)值 | P值 |
|---|---|---|---|---|
| PT( | 15.1±3.1 | 16.4±3.3 | -2.107 | 0.037 |
| INR( | 1.35±0.27 | 1.62±0.30 | -4.916 | <0.001 |
| APTT( | 57.20±17.74 | 67.04±22.08 | -2.537 | 0.013 |
| FIB( | 1.54±0.62 | 1.45±0.61 | 0.761 | 0.448 |
| DD[M(Q1,Q3),mg/L] | 4.409(1.734,4.283) | 5.049(1.987,6.311) | -0.595a | 0.553 |
表2 早产儿非GMH-IVH组与GMH-IVH组凝血功能指标比较
Table 2 Comparison of coagulation function between non-GMH-IVH group and GMH-IVH group
| 指标 | 非GMH-IVH组(n=55) | GMH-IVH组(n=51) | t(Z)值 | P值 |
|---|---|---|---|---|
| PT( | 15.1±3.1 | 16.4±3.3 | -2.107 | 0.037 |
| INR( | 1.35±0.27 | 1.62±0.30 | -4.916 | <0.001 |
| APTT( | 57.20±17.74 | 67.04±22.08 | -2.537 | 0.013 |
| FIB( | 1.54±0.62 | 1.45±0.61 | 0.761 | 0.448 |
| DD[M(Q1,Q3),mg/L] | 4.409(1.734,4.283) | 5.049(1.987,6.311) | -0.595a | 0.553 |
| 指标 | 非GMH-IVH组(n=55) | GMH-IVH组(n=51) | t值 | P值 |
|---|---|---|---|---|
| SBP | ||||
| 平均值(mmHg) | 57.02±5.79 | 56.08±6.31 | 0.800 | 0.426 |
| Max-min(mmHg) | 21.62±6.68 | 25.08±6.88 | -2.625 | 0.010 |
| SD(mmHg) | 5.27±1.49 | 6.12±1.72 | -2.739 | 0.007 |
| CV(%) | 9.58±2.96 | 11.18±3.68 | -2.468 | 0.015 |
| SV | 7.91±1.27 | 8.22±1.46 | -1.167 | 0.246 |
| DBP | ||||
| 平均值(mmHg) | 29.11±4.79 | 26.80±5.31 | 2.349 | 0.021 |
| Max-min(mmHg) | 21.65±6.92 | 25.84±5.91 | -3.337 | 0.001 |
| SD(mmHg) | 5.61±1.62 | 6.64±1.32 | -3.558 | 0.001 |
| CV(%) | 20.02±7.74 | 25.72±7.21 | -3.314 | 0.001 |
| SV | 7.24±1.19 | 7.68±1.45 | -1.705 | 0.090 |
表3 早产儿非GMH-IVH组与GMH-IVH组BPV指标比较(±s)
Table 3 Comparison of BPV between non-GMH-IVH group and GMH-IVH group
| 指标 | 非GMH-IVH组(n=55) | GMH-IVH组(n=51) | t值 | P值 |
|---|---|---|---|---|
| SBP | ||||
| 平均值(mmHg) | 57.02±5.79 | 56.08±6.31 | 0.800 | 0.426 |
| Max-min(mmHg) | 21.62±6.68 | 25.08±6.88 | -2.625 | 0.010 |
| SD(mmHg) | 5.27±1.49 | 6.12±1.72 | -2.739 | 0.007 |
| CV(%) | 9.58±2.96 | 11.18±3.68 | -2.468 | 0.015 |
| SV | 7.91±1.27 | 8.22±1.46 | -1.167 | 0.246 |
| DBP | ||||
| 平均值(mmHg) | 29.11±4.79 | 26.80±5.31 | 2.349 | 0.021 |
| Max-min(mmHg) | 21.65±6.92 | 25.84±5.91 | -3.337 | 0.001 |
| SD(mmHg) | 5.61±1.62 | 6.64±1.32 | -3.558 | 0.001 |
| CV(%) | 20.02±7.74 | 25.72±7.21 | -3.314 | 0.001 |
| SV | 7.24±1.19 | 7.68±1.45 | -1.705 | 0.090 |
| 变量 | B | SE | Wald χ2值 | P值 | OR(95%CI) |
|---|---|---|---|---|---|
| PROM | 0.357 | 0.553 | 2.415 | 0.519 | 1.528(0.483~3.224) |
| PT | 0.154 | 0.102 | 1.052 | 0.244 | 1.045(0.730~1.384) |
| INR | 2.929 | 0.992 | 8.711 | 0.003 | 5.608(2.858~8.587) |
| APTT | 0.021 | 0.016 | 0.107 | 0.909 | 1.028(0.972~1.603) |
| SBP | |||||
| Max-min | 0.011 | 0.044 | 0.062 | 0.826 | 1.010(0.927~1.099) |
| SD | 0.345 | 0.279 | 2.013 | 0.417 | 1.115(0.818~1.622) |
| CV | 0.132 | 0.176 | 0.567 | 0.451 | 1.052(0.809~1.611) |
| DBP | |||||
| 平均值 | -0.031 | 0.50 | 0.377 | 0.482 | 0.970(0.876~1.165) |
| Max-min | 0.002 | 0.044 | 0.003 | 0.908 | 1.109(0.922~1.295) |
| SD | 0.690 | 0.465 | 2.852 | 0.038 | 1.455(1.003~2.111) |
| CV | 0.305 | 0.191 | 1.195 | 0.139 | 1.093(0.800~1.962) |
表4 早产儿GMH-IVH危险因素的二元Logistic回归分析
Table 4 Binary Logistic regression analysis of risk factors for GMH-IVH
| 变量 | B | SE | Wald χ2值 | P值 | OR(95%CI) |
|---|---|---|---|---|---|
| PROM | 0.357 | 0.553 | 2.415 | 0.519 | 1.528(0.483~3.224) |
| PT | 0.154 | 0.102 | 1.052 | 0.244 | 1.045(0.730~1.384) |
| INR | 2.929 | 0.992 | 8.711 | 0.003 | 5.608(2.858~8.587) |
| APTT | 0.021 | 0.016 | 0.107 | 0.909 | 1.028(0.972~1.603) |
| SBP | |||||
| Max-min | 0.011 | 0.044 | 0.062 | 0.826 | 1.010(0.927~1.099) |
| SD | 0.345 | 0.279 | 2.013 | 0.417 | 1.115(0.818~1.622) |
| CV | 0.132 | 0.176 | 0.567 | 0.451 | 1.052(0.809~1.611) |
| DBP | |||||
| 平均值 | -0.031 | 0.50 | 0.377 | 0.482 | 0.970(0.876~1.165) |
| Max-min | 0.002 | 0.044 | 0.003 | 0.908 | 1.109(0.922~1.295) |
| SD | 0.690 | 0.465 | 2.852 | 0.038 | 1.455(1.003~2.111) |
| CV | 0.305 | 0.191 | 1.195 | 0.139 | 1.093(0.800~1.962) |
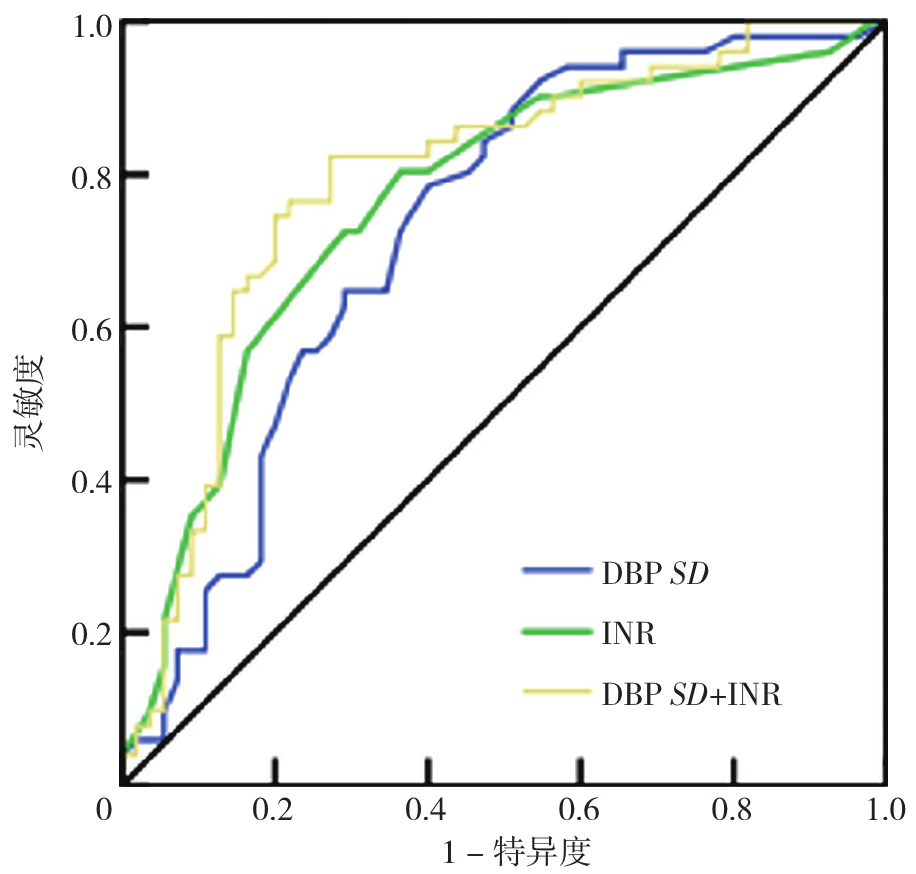
图1 INR、DBP的SD及两者联合预测早产儿GMH-IVH的ROC曲线注:DBP SD=舒张压的标准差,INR=国际标准化比值,DBP SD+INR=两者联合
Figure 1 ROC curve of INR, SD of DBP and the combination of both for predicting GMH-IVH
| 指标 | AUC(95%CI) | 最佳截断值 | P值 | 灵敏度(%) | 特异度(%) | 约登指数 |
|---|---|---|---|---|---|---|
| INR | 0.764(0.671~0.856) | 1.565 | <0.001 | 72.5 | 70.9 | 0.434 |
| DBP的SD | 0.727(0.629~0.824) | 5.750 | <0.001 | 78.4 | 68.5 | 0.469 |
| 两者联合 | 0.803(0.724~0.881) | 0.405 | <0.001 | 82.4 | 79.7 | 0.621 |
表5 INR、DBP的SD及两者联合对早产儿GMH-IVH的预测价值
Table 5 To evaluate the predictive value of INR, SD of DBP and their combination for GMH-IVH in preterm infants
| 指标 | AUC(95%CI) | 最佳截断值 | P值 | 灵敏度(%) | 特异度(%) | 约登指数 |
|---|---|---|---|---|---|---|
| INR | 0.764(0.671~0.856) | 1.565 | <0.001 | 72.5 | 70.9 | 0.434 |
| DBP的SD | 0.727(0.629~0.824) | 5.750 | <0.001 | 78.4 | 68.5 | 0.469 |
| 两者联合 | 0.803(0.724~0.881) | 0.405 | <0.001 | 82.4 | 79.7 | 0.621 |
| 指标 | 转归良好组(n=30) | 转归不良组(n=21) | t(Z)值 | P值 |
|---|---|---|---|---|
| PT( | 16.1±2.9 | 16.8±3.7 | -0.675 | 0.503 |
| INR( | 1.53±0.25 | 1.74±0.34 | -2.489 | 0.016 |
| APTT( | 61.3±19.8 | 75.2±23.1 | -2.298 | 0.026 |
| FIB( | 1.56±0.61 | 1.28±0.57 | 1.651 | 0.105 |
| DD[M(Q1,Q3),mg/L] | 4.823(1.875,6.325) | 5.372(2.116,6.528) | -0.368a | 0.715 |
表6 GMH-IVH转归良好组与转归不良组凝血指标比较
Table 6 Comparison of coagulation between the good outcome group and the poor outcome group of GMH-IVH
| 指标 | 转归良好组(n=30) | 转归不良组(n=21) | t(Z)值 | P值 |
|---|---|---|---|---|
| PT( | 16.1±2.9 | 16.8±3.7 | -0.675 | 0.503 |
| INR( | 1.53±0.25 | 1.74±0.34 | -2.489 | 0.016 |
| APTT( | 61.3±19.8 | 75.2±23.1 | -2.298 | 0.026 |
| FIB( | 1.56±0.61 | 1.28±0.57 | 1.651 | 0.105 |
| DD[M(Q1,Q3),mg/L] | 4.823(1.875,6.325) | 5.372(2.116,6.528) | -0.368a | 0.715 |
| 指标 | 转归良好组(n=30) | 转归不良组(n=21) | t值 | P值 |
|---|---|---|---|---|
| SBP | ||||
| 平均值(mmHg) | 56.63±6.64 | 55.29±5.88 | 0.747 | 0.459 |
| Max-min(mmHg) | 24.80±6.18 | 25.48±7.93 | -0.342 | 0.734 |
| SD(mmHg) | 5.74±1.73 | 6.75±1.56 | -2.139 | 0.037 |
| CV(%) | 10.13±3.61 | 12.33±3.20 | -2.243 | 0.029 |
| SV | 8.08±1.65 | 8.43±1.14 | -0.846 | 0.402 |
| DBP | ||||
| 平均值(mmHg) | 27.97±6.12 | 24.90±3.55 | 2.059 | 0.045 |
| Max-min(mmHg) | 24.87±6.21 | 27.24±5.29 | -1.425 | 0.161 |
| SD(mmHg) | 6.14±1.22 | 7.38±1.10 | -3.710 | 0.001 |
| CV(%) | 23.43±6.75 | 29.21±6.70 | -3.022 | 0.004 |
| SV | 7.37±1.53 | 8.12±1.25 | -1.857 | 0.069 |
表7 GMH-IVH转归良好组与转归不良组BPV指标比较(±s)
Table 7 Comparison of BPV between the good outcome group and the poor outcome group of GMH-IVH
| 指标 | 转归良好组(n=30) | 转归不良组(n=21) | t值 | P值 |
|---|---|---|---|---|
| SBP | ||||
| 平均值(mmHg) | 56.63±6.64 | 55.29±5.88 | 0.747 | 0.459 |
| Max-min(mmHg) | 24.80±6.18 | 25.48±7.93 | -0.342 | 0.734 |
| SD(mmHg) | 5.74±1.73 | 6.75±1.56 | -2.139 | 0.037 |
| CV(%) | 10.13±3.61 | 12.33±3.20 | -2.243 | 0.029 |
| SV | 8.08±1.65 | 8.43±1.14 | -0.846 | 0.402 |
| DBP | ||||
| 平均值(mmHg) | 27.97±6.12 | 24.90±3.55 | 2.059 | 0.045 |
| Max-min(mmHg) | 24.87±6.21 | 27.24±5.29 | -1.425 | 0.161 |
| SD(mmHg) | 6.14±1.22 | 7.38±1.10 | -3.710 | 0.001 |
| CV(%) | 23.43±6.75 | 29.21±6.70 | -3.022 | 0.004 |
| SV | 7.37±1.53 | 8.12±1.25 | -1.857 | 0.069 |
| 变量 | B | SE | Wald χ2值 | P值 | OR(95%CI) |
|---|---|---|---|---|---|
| INR | 3.350 | 1.499 | 4.922 | 0.025 | 3.942(1.509~6.680) |
| APTT | 0.009 | 0.022 | 0.157 | 0.692 | 1.041(0.949~1.136) |
| SBP | |||||
| SD | 0.022 | 0.279 | 0.006 | 0.938 | 1.022(0.592~1.765) |
| CV | 0.267 | 0.329 | 0.660 | 0.417 | 1.306(0.686~2.488) |
| DBP | |||||
| 平均值 | -0.109 | 0.090 | 1.477 | 0.224 | 0.897(0.752~1.369) |
| SD | 0.848 | 0.426 | 3.962 | 0.047 | 2.334(1.013~5.378) |
| CV | 0.555 | 0.296 | 3.519 | 0.061 | 1.723(0.975~3.113) |
表8 早产儿GMH-IVH转归不良危险因素的二元Logistic回归分析
Table 8 Risk factors for poor outcomes of GMH-IVH were analyzed by binary Logistic regression
| 变量 | B | SE | Wald χ2值 | P值 | OR(95%CI) |
|---|---|---|---|---|---|
| INR | 3.350 | 1.499 | 4.922 | 0.025 | 3.942(1.509~6.680) |
| APTT | 0.009 | 0.022 | 0.157 | 0.692 | 1.041(0.949~1.136) |
| SBP | |||||
| SD | 0.022 | 0.279 | 0.006 | 0.938 | 1.022(0.592~1.765) |
| CV | 0.267 | 0.329 | 0.660 | 0.417 | 1.306(0.686~2.488) |
| DBP | |||||
| 平均值 | -0.109 | 0.090 | 1.477 | 0.224 | 0.897(0.752~1.369) |
| SD | 0.848 | 0.426 | 3.962 | 0.047 | 2.334(1.013~5.378) |
| CV | 0.555 | 0.296 | 3.519 | 0.061 | 1.723(0.975~3.113) |
| 指标 | AUC(95%CI) | 最佳截断值 | P值 | 灵敏度(%) | 特异度(%) | 约登指数 |
|---|---|---|---|---|---|---|
| INR | 0.808(0.683~0.933) | 1.850 | 0.001 | 61.9 | 96.7 | 0.586 |
| DBP的SD | 0.773(0.645~0.901) | 6.650 | <0.001 | 81.0 | 66.7 | 0.477 |
| 两者联合 | 0.864(0.760~0.968) | 0.541 | <0.001 | 76.2 | 90.0 | 0.662 |
表9 INR、DBP的SD及两者联合对早产儿GMH-IVH转归不良的预测价值
Table 9 Predictive value of INR, SD of DBP and their combination for poor outcomes of GMH-IVH
| 指标 | AUC(95%CI) | 最佳截断值 | P值 | 灵敏度(%) | 特异度(%) | 约登指数 |
|---|---|---|---|---|---|---|
| INR | 0.808(0.683~0.933) | 1.850 | 0.001 | 61.9 | 96.7 | 0.586 |
| DBP的SD | 0.773(0.645~0.901) | 6.650 | <0.001 | 81.0 | 66.7 | 0.477 |
| 两者联合 | 0.864(0.760~0.968) | 0.541 | <0.001 | 76.2 | 90.0 | 0.662 |
| [1] |
|
| [2] |
|
| [3] |
|
| [4] |
|
| [5] |
|
| [6] |
|
| [7] |
|
| [8] |
|
| [9] |
|
| [10] |
|
| [11] |
|
| [12] |
|
| [13] |
|
| [14] |
|
| [15] |
|
| [16] |
|
| [17] |
|
| [18] |
|
| [19] |
|
| [20] |
|
| [21] |
|
| [22] |
|
| [23] |
|
| [24] |
|
| [25] |
|
| [26] |
|
| [27] |
|
| [28] |
|
| [29] |
|
| [30] |
|
| [31] |
|
| [1] | 邱欣雨, 赵倩, 陈玉斐, 加木勒·买买提依明, 韩聪聪, 爱克丹·艾尔肯, 李晓梅, 杨毅宁. 体重状态及其代谢特征对收缩压纵向轨迹的影响:一项队列研究[J]. 中国全科医学, 2026, 29(15): 2006-2013. |
| [2] | 刘帆, 陈秋雨, 李婧. 亚临床高风险人群夜间高血压筛查模型的构建与验证:一项单中心队列研究[J]. 中国全科医学, 2026, 29(15): 1998-2005. |
| [3] | 刘天缘, 桑婉玥, 彭继平, 程思怡, 黄伊伊, 李欧文, 江洪, 周晓亚. 神经丝轻链蛋白与夜间高血压患者左心室肥厚发生风险的相关性研究[J]. 中国全科医学, 2026, 29(15): 2014-2021. |
| [4] | 王斯曼, 张梦楚, 李文, 许艾, 徐璡, 郭睿, 燕海霞. 基于中医证候及脉图参数构建原发性高血压伴左心室肥厚风险预测模型研究[J]. 中国全科医学, 2026, 29(14): 1840-1848. |
| [5] | 吴春香, 田婕, 郭毅, 邓波, 于杰, 蔡宁, 沈莉. 高血压患者8年就医行为轨迹及影响因素分析[J]. 中国全科医学, 2026, 29(13): 1660-1665. |
| [6] | 宋路, 王丽晔, 修春霞, 冯宝静, 冯丽萍, 高艳松, 李梦, 代妍. 慢性阻塞性肺疾病合并高血压患者肺功能与血压变异性的相关研究[J]. 中国全科医学, 2026, 29(10): 1311-1315. |
| [7] | 焦玺同, 刘璐, 郭嘉悦, 尤莉莉. 国内外高血压数字疗法产品的应用前景及对我国的启示[J]. 中国全科医学, 2026, 29(10): 1354-1360. |
| [8] | 张秋雨, 胡晓咏, 唐瑞, 李红建. 中国人内脏脂肪指数与中青年夜间高血压的相关性研究[J]. 中国全科医学, 2026, 29(07): 872-878. |
| [9] | 李杰, 杨昕晖, 曹黎, 张晶, 姜岳. 一例"三高"合并脂肪性肝病患者的全科诊疗案例分析[J]. 中国全科医学, 2026, 29(06): 810-816. |
| [10] | 雷莹莹, 郑锶颖, 汪文新, 姜虹. 1990—2021年全球及中国高血压心脏病流行趋势及预测研究[J]. 中国全科医学, 2026, 29(05): 641-648. |
| [11] | 鹿妍秋, 吴云涛, 刘少鹏, 林海颖, 邓惠友, 武英, 黄喆, 杨鹏, 吴寿岭, 李云. 正常高值血压人群血压轨迹对心血管疾病发病风险的影响:基于开滦队列研究[J]. 中国全科医学, 2026, 29(03): 299-310. |
| [12] | 周文超, 梁佳琪, 姚尚满, 薛朝, 刘龙, 郭相杰. 高血压与帕金森病的共享基因位点识别研究[J]. 中国全科医学, 2026, 29(02): 201-206. |
| [13] | 闵叶平, 薛垚, 冯同保, 张合, 刘福菁. 血压反应指数对老年重症肺炎休克患者急性肾损伤的影响研究[J]. 中国全科医学, 2026, 29(02): 207-212. |
| [14] | 聂倩倩, 程桂荣, 宋丹, 李景耀, 许浪, 张丽娟. 中国社区老年人患高血压及其共病与痴呆的关联性研究[J]. 中国全科医学, 2026, 29(01): 76-83. |
| [15] | 陈玉斐, 赵倩, 谢依热·哈木拉提, 蔡丽婷, 李晓梅, 杨毅宁, 刘芬. 新疆阿勒泰地区农牧区人群"生命八要素"评分与高血压患病风险的横断面研究[J]. 中国全科医学, 2026, 29(01): 91-99. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||





