

Chinese General Practice ›› 2026, Vol. 29 ›› Issue (12): 1607-1617.DOI: 10.12114/j.issn.1007-9572.2024.0105
• Article • Previous Articles Next Articles
Received:2025-01-10
Revised:2025-08-25
Published:2026-04-20
Online:2026-03-12
Contact:
DING Xiaoqiang, SONG Nana
通讯作者:
丁小强, 宋娜娜
作者简介:作者贡献:
丁小强、宋娜娜提出研究设想;陈安南、颜芷昕、张健、沈波参与实验设计,负责实验实施,观测指标的测量,数据收集和统计学分析;陈安南、宋娜娜负责撰写文章初稿;丁小强、宋娜娜负责文章的质量控制和审校;所有作者确认了最终稿。
基金资助:CLC Number:
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.chinagp.net/EN/10.12114/j.issn.1007-9572.2024.0105
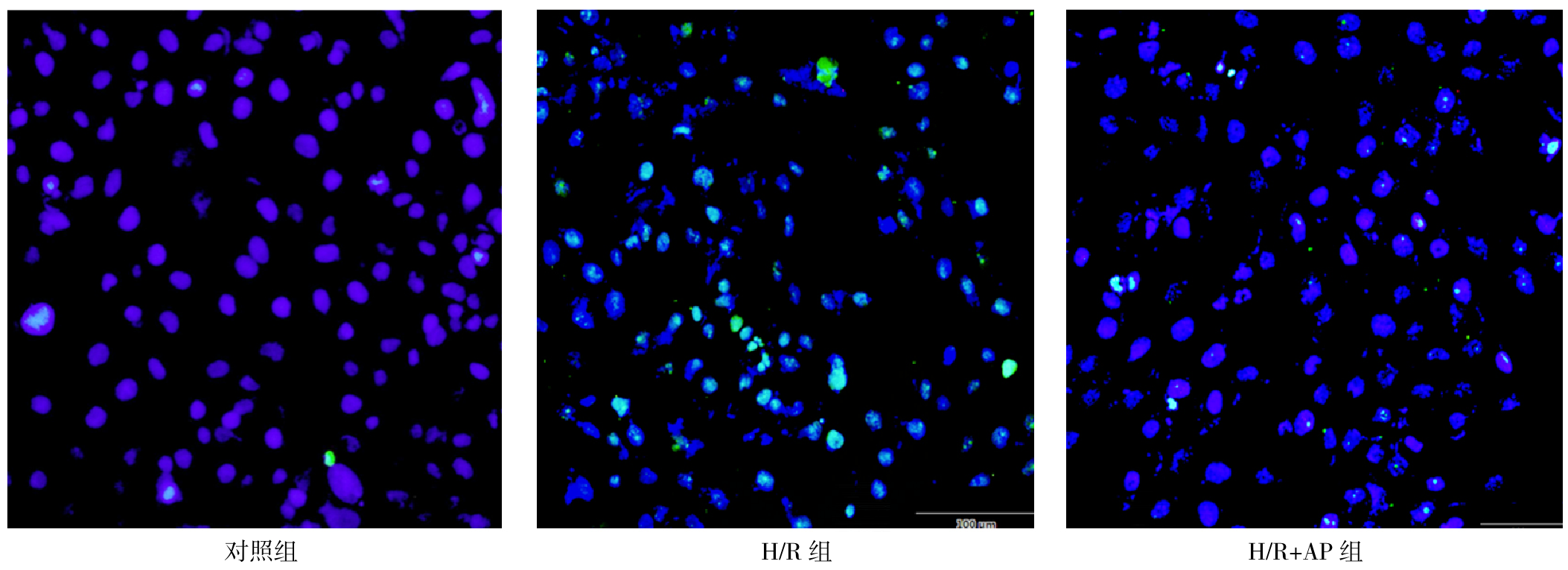
Figure 2 Results of Tunel staining of HK2 cells after H/R injury,when the acidic medium treatment time is 12 h and the normal medium recovery time is 6 h
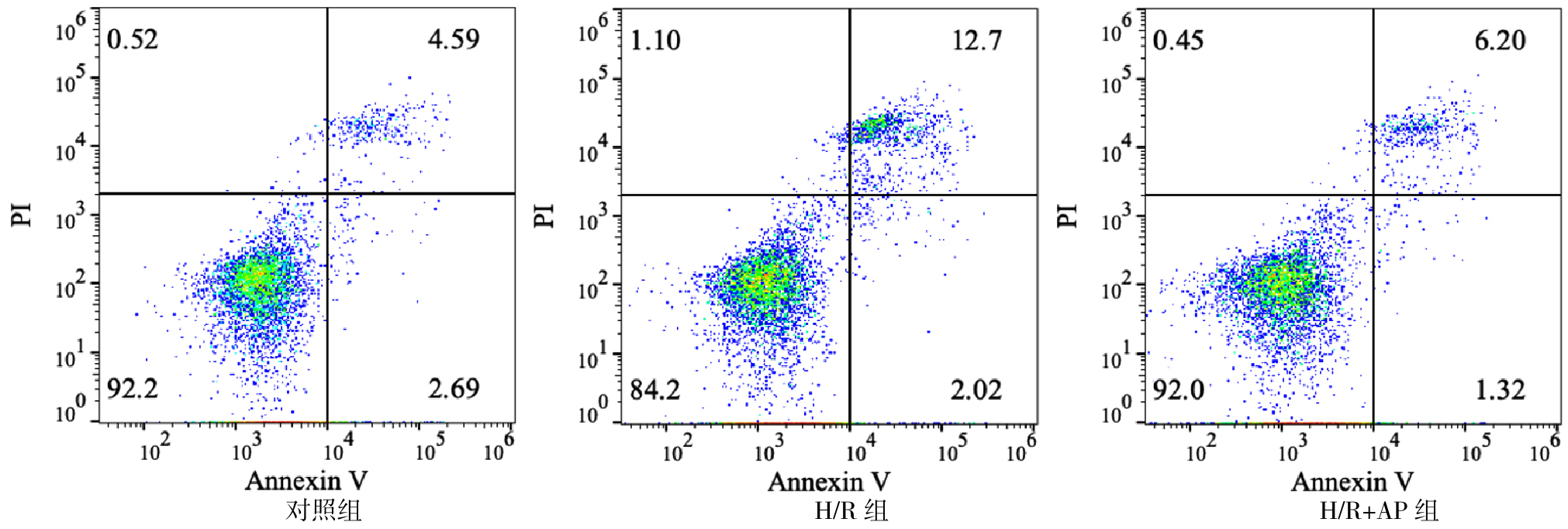
Figure 3 Results of Annexin V/PI detection of HK2 cells after H/R injury when the acidic medium treatment time is 12 h and the normal medium recovery time is 6 h
| 组别 | 只数 | 细胞活力 |
|---|---|---|
| 对照组 | 6 | 96.911±7.909 |
| H/R组 | 6 | 9.364±1.304a |
| H/R+A1R3组 | 6 | 13.810±3.078 |
| H/R+A6R3组 | 6 | 10.620±1.583 |
| H/R+A12R3组 | 6 | 19.638±3.502ab |
| H/R+A24R3组 | 6 | 11.132±1.405 |
| H/R+A12R6组 | 6 | 35.595±4.664bc |
| H/R+A12R12组 | 6 | 7.642±1.676 |
| F值 | 380.281 | |
| P值 | <0.001 |
Table 1 Comparison of cell viability of HK2 cells treated with A and R at different times after H/R injury
| 组别 | 只数 | 细胞活力 |
|---|---|---|
| 对照组 | 6 | 96.911±7.909 |
| H/R组 | 6 | 9.364±1.304a |
| H/R+A1R3组 | 6 | 13.810±3.078 |
| H/R+A6R3组 | 6 | 10.620±1.583 |
| H/R+A12R3组 | 6 | 19.638±3.502ab |
| H/R+A24R3组 | 6 | 11.132±1.405 |
| H/R+A12R6组 | 6 | 35.595±4.664bc |
| H/R+A12R12组 | 6 | 7.642±1.676 |
| F值 | 380.281 | |
| P值 | <0.001 |
| 组别 | 只数 | cleaved caspase 3 | cleaved caspase 9 |
|---|---|---|---|
| 对照组 | 4 | 1.198±0.462 | 1.061±0.169 |
| H/R组 | 4 | 4.620±0.283a | 2.865±0.441a |
| H/R+A1R3组 | 4 | 4.337±0.363 | 2.583±0.393 |
| H/R+A6R3组 | 4 | 3.953±0.410 | 2.402±0.335 |
| H/R+A12R3组 | 4 | 2.422±0.176ab | 1.460±0.287ab |
| H/R+A24R3组 | 4 | 3.968±0.715 | 3.006±0.712 |
| H/R+A48R3组 | 4 | 4.389±0.763 | 2.973±0.425 |
| H/R+A12R0组 | 4 | 4.377±0.386 | 4.781±0.551 |
| H/R+A12R6组 | 4 | 1.740±0.285ac | 2.099±0.260ac |
| H/R+A12R9组 | 4 | 3.545±0.250 | 3.545±0.157 |
| H/R+A12R12组 | 4 | 3.726±0.523 | 4.405±0.417 |
| F值 | 19.673 | 22.786 | |
| P值 | <0.001 | <0.001 |
Table 2 Expression of cleaved caspase 3 and cleaved caspase 9 protein in HK2 cells treated with A and R at different time points after H/R injury
| 组别 | 只数 | cleaved caspase 3 | cleaved caspase 9 |
|---|---|---|---|
| 对照组 | 4 | 1.198±0.462 | 1.061±0.169 |
| H/R组 | 4 | 4.620±0.283a | 2.865±0.441a |
| H/R+A1R3组 | 4 | 4.337±0.363 | 2.583±0.393 |
| H/R+A6R3组 | 4 | 3.953±0.410 | 2.402±0.335 |
| H/R+A12R3组 | 4 | 2.422±0.176ab | 1.460±0.287ab |
| H/R+A24R3组 | 4 | 3.968±0.715 | 3.006±0.712 |
| H/R+A48R3组 | 4 | 4.389±0.763 | 2.973±0.425 |
| H/R+A12R0组 | 4 | 4.377±0.386 | 4.781±0.551 |
| H/R+A12R6组 | 4 | 1.740±0.285ac | 2.099±0.260ac |
| H/R+A12R9组 | 4 | 3.545±0.250 | 3.545±0.157 |
| H/R+A12R12组 | 4 | 3.726±0.523 | 4.405±0.417 |
| F值 | 19.673 | 22.786 | |
| P值 | <0.001 | <0.001 |
| 组别 | 只数 | Tunel阳性细胞比例 | Annexin V阳性细胞比例 |
|---|---|---|---|
| 对照组 | 4 | 0.811±0.201 | 4.882±1.099 |
| H/R组 | 4 | 55.348±2.585a | 26.268±5.151a |
| H/R+AP组 | 4 | 21.716±3.404b | 9.986±1.050b |
| F值 | 124.042 | 14.066 | |
| P值 | <0.001 | <0.001 |
Table 3 The proportion of Tunel-positive cells and the proportion of Annexin V-positive cells in HK2 cells after H/R injury when the acidic medium treatment time is 12 h and the normal medium recovery time is 6 h
| 组别 | 只数 | Tunel阳性细胞比例 | Annexin V阳性细胞比例 |
|---|---|---|---|
| 对照组 | 4 | 0.811±0.201 | 4.882±1.099 |
| H/R组 | 4 | 55.348±2.585a | 26.268±5.151a |
| H/R+AP组 | 4 | 21.716±3.404b | 9.986±1.050b |
| F值 | 124.042 | 14.066 | |
| P值 | <0.001 | <0.001 |
| 组别 | 只数 | pHi |
|---|---|---|
| 对照组 | 4 | 7.304±0.031 |
| H/R组 | 4 | 6.842±0.041a |
| H/R+AP组 | 4 | 7.000±0.094b |
| F值 | 85.577 | |
| P值 | <0.001 |
Table 4 pHi of AP-treated HK2 cells before and after H/R injury
| 组别 | 只数 | pHi |
|---|---|---|
| 对照组 | 4 | 7.304±0.031 |
| H/R组 | 4 | 6.842±0.041a |
| H/R+AP组 | 4 | 7.000±0.094b |
| F值 | 85.577 | |
| P值 | <0.001 |
| 组别 | 只数 | NHE1活性(dpHi/dt) | NHE1表达量 |
|---|---|---|---|
| Scramble组 | 3 | 0.133±0.017 | 0.997±0.028 |
| siNHE1组 | 3 | 0.021±0.003a | 0.309±0.042a |
| AP组 | 3 | 0.240±0.003ab | 3.393±1.537ab |
| AP+siNHE1组 | 3 | 0.031±0.021ac | 0.330±0.032ac |
| F值 | 41.811 | 14.135 | |
| P值 | <0.001 | <0.001 |
Table 5 NHE1 activity of HK2 cells after knockdown of NHE1 expression
| 组别 | 只数 | NHE1活性(dpHi/dt) | NHE1表达量 |
|---|---|---|---|
| Scramble组 | 3 | 0.133±0.017 | 0.997±0.028 |
| siNHE1组 | 3 | 0.021±0.003a | 0.309±0.042a |
| AP组 | 3 | 0.240±0.003ab | 3.393±1.537ab |
| AP+siNHE1组 | 3 | 0.031±0.021ac | 0.330±0.032ac |
| F值 | 41.811 | 14.135 | |
| P值 | <0.001 | <0.001 |
| 组别 | 只数 | cleaved caspase 3 | cleaved caspase 9 | NHE1 |
|---|---|---|---|---|
| 对照组 | 4 | 1.000±0.081 | 1.000±0.072 | 1.000±0.048 |
| siNHE1组 | 4 | 0.859±0.274 | 0.931±0.400 | 0.311±0.039 |
| H/R组 | 4 | 5.264±0.635a | 6.982±0.439a | 1.219±0.173 |
| AP组 | 4 | 1.127±0.257 | 1.026±0.171b | 3.036±0.642 |
| AP+siNHE1组 | 4 | 1.307±0.369 | 1.102±0.072b | 0.372±0.087 |
| H/R+ siNHE1组 | 4 | 4.641±0.434a | 6.561±0.459a | 0.417±0.093 |
| H/R+AP组 | 4 | 1.854±0.492ab | 3.711±0.754ab | 3.258±0.629 |
| H/R+AP+ siNHE1组 | 4 | 4.075±0.422ac | 5.612±0.216ac | 0.401±0.064 |
| F值 | 82.539 | 190.997 | 65.973 | |
| P值 | <0.001 | <0.001 | <0.001 |
Table 6 Expression of NHE1,cleaved caspase 3 and cleaved caspase 9 protein in HK2 cells treated with AP and siNHE1 after H/R injury
| 组别 | 只数 | cleaved caspase 3 | cleaved caspase 9 | NHE1 |
|---|---|---|---|---|
| 对照组 | 4 | 1.000±0.081 | 1.000±0.072 | 1.000±0.048 |
| siNHE1组 | 4 | 0.859±0.274 | 0.931±0.400 | 0.311±0.039 |
| H/R组 | 4 | 5.264±0.635a | 6.982±0.439a | 1.219±0.173 |
| AP组 | 4 | 1.127±0.257 | 1.026±0.171b | 3.036±0.642 |
| AP+siNHE1组 | 4 | 1.307±0.369 | 1.102±0.072b | 0.372±0.087 |
| H/R+ siNHE1组 | 4 | 4.641±0.434a | 6.561±0.459a | 0.417±0.093 |
| H/R+AP组 | 4 | 1.854±0.492ab | 3.711±0.754ab | 3.258±0.629 |
| H/R+AP+ siNHE1组 | 4 | 4.075±0.422ac | 5.612±0.216ac | 0.401±0.064 |
| F值 | 82.539 | 190.997 | 65.973 | |
| P值 | <0.001 | <0.001 | <0.001 |
| 组别 | 只数 | NHE1表达量 | NHE1活性(dpHi/dt) |
|---|---|---|---|
| 对照组 | 4 | 1.000±0.154 | 0.387±0.036 |
| AP组 | 4 | 5.072±0.164a | 0.685±0.207a |
| 低氯培养组 | 4 | 0.925±0.157b | 0.381±0.059b |
| AP+低氯培养组 | 4 | 1.318±0.277b | 0.388±0.049b |
| F值 | 422.575 | 5.371 | |
| P值 | <0.001 | 0.026 |
Table 7 Expression of NHE1 protein in HK2 cells cultured in low chlorine solution after AP
| 组别 | 只数 | NHE1表达量 | NHE1活性(dpHi/dt) |
|---|---|---|---|
| 对照组 | 4 | 1.000±0.154 | 0.387±0.036 |
| AP组 | 4 | 5.072±0.164a | 0.685±0.207a |
| 低氯培养组 | 4 | 0.925±0.157b | 0.381±0.059b |
| AP+低氯培养组 | 4 | 1.318±0.277b | 0.388±0.049b |
| F值 | 422.575 | 5.371 | |
| P值 | <0.001 | 0.026 |
| 组别 | 只数 | NHE1 | cleaved caspase 3 | KIM1 |
|---|---|---|---|---|
| sham组 | 6 | 1.044±0.103 | 1.000±0.151 | 1.000±0.285 |
| IPC组 | 6 | 1.041±0.392a | 2.858±0.369 | 0.859±0.285 |
| I/R组 | 6 | 1.774±0.392 | 3.580±0.413a | 9.797±0.954a |
| IPC+I/R组 | 6 | 2.858±0.485b | 1.828±0.489b | 3.868±0.345b |
| F值 | 39.265 | 60.199 | 323.384 | |
| P值 | <0.001 | <0.001 | <0.001 |
Table 8 Expression of NHE1,KIM1 and cleaved caspase3 protein in mices treated with IPC after I/R
| 组别 | 只数 | NHE1 | cleaved caspase 3 | KIM1 |
|---|---|---|---|---|
| sham组 | 6 | 1.044±0.103 | 1.000±0.151 | 1.000±0.285 |
| IPC组 | 6 | 1.041±0.392a | 2.858±0.369 | 0.859±0.285 |
| I/R组 | 6 | 1.774±0.392 | 3.580±0.413a | 9.797±0.954a |
| IPC+I/R组 | 6 | 2.858±0.485b | 1.828±0.489b | 3.868±0.345b |
| F值 | 39.265 | 60.199 | 323.384 | |
| P值 | <0.001 | <0.001 | <0.001 |
| 组别 | 只数 | 肾脏组织pH | 肾脏细胞pHi |
|---|---|---|---|
| sham组 | 4 | 7.389±0.096 | 7.476±0.103 |
| I/R组 | 4 | 6.073±0.096a | 7.286±0.073a |
| IPC+I/R组 | 4 | 6.088±0.169 | 7.304±0.031b |
| F值 | 17.386 | 10.521 | |
| P值 | <0.001 | <0.001 |
Table 9 pH of mice kidney tissue and pHi of mice kidney cells
| 组别 | 只数 | 肾脏组织pH | 肾脏细胞pHi |
|---|---|---|---|
| sham组 | 4 | 7.389±0.096 | 7.476±0.103 |
| I/R组 | 4 | 6.073±0.096a | 7.286±0.073a |
| IPC+I/R组 | 4 | 6.088±0.169 | 7.304±0.031b |
| F值 | 17.386 | 10.521 | |
| P值 | <0.001 | <0.001 |
| [1] |
|
| [2] |
|
| [3] |
|
| [4] |
|
| [5] |
|
| [6] |
|
| [7] |
|
| [8] |
|
| [9] |
陈安南, 丁小强, 宋娜娜. Na+/H+交换体1在肾脏疾病中的作用[J]. 中国病理生理杂志, 2023, 39(4): 721-729. DOI: 10.3969/j.issn.1000-4718.2023.04.018.
|
| [10] |
|
| [11] |
|
| [12] |
|
| [13] |
|
| [14] |
|
| [15] |
|
| [16] |
|
| [17] |
|
| [18] |
|
| [19] |
|
| [20] |
|
| [21] |
|
| [1] | WANG Tingting, LIN Zehua, MA Yingchun, Committee of Kidney Disease Rehabilitation, Chinese Association of Rehabilitation Medicine. Specification of Rehabilitation Service for Elderly Patients with Comorbidity Complicated with Acute Kidney Injury [J]. Chinese General Practice, 2026, 29(11): 1361-1366. |
| [2] | MIN Yeping, XUE Yao, FENG Tongbao, ZHANG He, LIU Fujing. Effect of Blood Pressure Response Index on Acute Kidney Injury in Elderly Patients with Severe Pneumonia Shock [J]. Chinese General Practice, 2026, 29(02): 207-212. |
| [3] | WANG Xiaoyu, FENG Zhenzhen, WANG Jun, GUO Xiaochuan, LI Jiansheng. Risk Factors for Acute Kidney Injury in Acute Respiratory Distress Syndrome: a Systematic Review [J]. Chinese General Practice, 2025, 28(12): 1527-1537. |
| [4] | ZHANG Pei, YANG Meng, GAO Chunlin, XIA Zhengkun. Study on the Intervention and Prognosis of Modified Lifting Powder on Acute Kidney Injury and Acute Kidney Disease in Children [J]. Chinese General Practice, 2025, 28(11): 1376-1382. |
| [5] | WANG Linna, ZHANG Jinghui. Expression and Prognostic Value of Serum SAA, IL-6, TNF-α and microRNAs in Children with Sepsis Complicated with Acute Kidney Injury [J]. Chinese General Practice, 2025, 28(03): 293-298. |
| [6] | TILAKEZI Tuersun, WEI Haiyan, NUERBAHAER Remutula, YANG Heyin. Diagnostic Value of Serum NLRP3 Levels and Contrast Agent Dosage in Contrast-induced Nephropathy after Percutaneous Coronary Intervention in Patients with Acute ST-elevation Myocardial Infarction [J]. Chinese General Practice, 2024, 27(27): 3378-3382. |
| [7] | LIU Xiaogang, YANG Shicheng, FU Naikuan, SHAO Dujing, ZHANG Peng. The Impact of Dapagliflozin on the Incidence of Contrast-induced Nephropathy in Patients with Type 2 Diabetes Mellitus Underwent Percutaneous Coronary Intervention [J]. Chinese General Practice, 2024, 27(24): 2994-2999. |
| [8] | PEI Xuejing, SHEN Huaiyun, XU Qianqian, LIU Binbin, WANG Huihui. Risk Factors and Short-term Prognosis of Severe Neonatal Asphyxia Complicated with Acute Kidney Injury [J]. Chinese General Practice, 2024, 27(15): 1861-1866. |
| [9] | WANG Zhen, SHEN Guoqi, LI Yanan, ZHU Yinghua, QIU Hang, ZHENG Di, XU Tongda, LI Wenhua. Development and Validation of a Risk Prediction Model for Contrast-induced Acute Kidney Injury after Percutaneous Coronary Intervention in Patients with Acute Myocardial Infarction [J]. Chinese General Practice, 2023, 26(29): 3650-3656. |
| [10] | WANG Xiaowen, XIAO Tongling, WANG Yi, YANG Ying, XIA Xiaoshuang, LI Xin. Relationship between Homocysteine Level and Acute Kidney Injury in Patients with Acute Ischemic Stroke [J]. Chinese General Practice, 2023, 26(26): 3290-3296. |
| [11] | YAN Peng, SONG Jianling, FANG Xiangdong. Recent Developments in Parathyroid Hormone Type 1 Receptor and Kidney Disease [J]. Chinese General Practice, 2023, 26(11): 1398-1403. |
| [12] | XU Wei, XU Jiyuan, LI Maoqin, LU Fei, CHENG Shuli. Predictive Value of Color Doppler Ultrasound for Acute Kidney Injury in Patients with Septic Shock [J]. Chinese General Practice, 2023, 26(09): 1104-1111. |
| [13] | Meiying CHEN, Muxin CHEN, Mingxin WANG, Chanmei ZHENG, Wanzhu CAI, Aixin LIANG, Chunjiao ZHOU. Risk Factors for Acute Kidney Injury in Severe Acute Pancreatitis: a Meta-analysis [J]. Chinese General Practice, 2022, 25(30): 3834-3842. |
| [14] | Yan RAO, Meiqi YAO, Dawei JIANG, Cui MAO. Development and Validation of a Risk Prediction Model of Post-stroke Acute Kidney Injury [J]. Chinese General Practice, 2022, 25(23): 2885-2891. |
| [15] | Jinxiang WANG, Yuxin DONG, Yibo ZHAO, Xianglong MENG, Yanfen CHAI, Heng JIN. Advances in Diagnosis and Management of Acute Kidney Injury Induced by Crush Syndrome [J]. Chinese General Practice, 2022, 25(15): 1914-1918. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||