

Chinese General Practice ›› 2022, Vol. 25 ›› Issue (08): 963-968.DOI: 10.12114/j.issn.1007-9572.2021.01.414
Special Issue: 儿科最新文章合辑
• Original Research • Previous Articles Next Articles
Predictive Value of Hemodynamic Indicators for Bronchopulmonary Dysplasia in Preterm Infants
1.The Fourth Clinical College of Xinxiang Medical University,Xinxiang 453000,China
2.Xinxiang Central Hospital,Xinxiang 453000,China
*Corresponding author:ZHANG Weixing,Chief physician;E-mail:zhangweixing0420@126.com
Received:2021-12-08
Revised:2021-12-17
Published:2022-03-15
Online:2022-03-02
通讯作者:
张卫星
基金资助:CLC Number:
JIA Nan, HE Yujuan, ZHAO Xiaoxiao, ZHANG Weixing.
Predictive Value of Hemodynamic Indicators for Bronchopulmonary Dysplasia in Preterm Infants [J]. Chinese General Practice, 2022, 25(08): 963-968.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.chinagp.net/EN/10.12114/j.issn.1007-9572.2021.01.414
| 组别 | 例数 | 胎龄(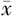 ±s,周) ±s,周) | 出生体质量(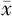 ±s,kg) ±s,kg) | 性别(男/女) | 分娩方式(顺/剖) |
|---|---|---|---|---|---|
| 对照组 | 96 | 29.5±1.4 | 1.27±0.19 | 49/47 | 51/45 |
| BPD组 | 65 | 29.0±1.5 | 1.23±0.21 | 29/36 | 29/36 |
| χ2(t)值 | -1.833a | -1.334a | 0.063 | 0.083 | |
| P值 | 0.069 | 0.184 | 0.423 | 0.289 |
Table 1 Comparison of general information between preterm infants with and without bronchopulmonary dysplasia
| 组别 | 例数 | 胎龄(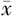 ±s,周) ±s,周) | 出生体质量(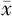 ±s,kg) ±s,kg) | 性别(男/女) | 分娩方式(顺/剖) |
|---|---|---|---|---|---|
| 对照组 | 96 | 29.5±1.4 | 1.27±0.19 | 49/47 | 51/45 |
| BPD组 | 65 | 29.0±1.5 | 1.23±0.21 | 29/36 | 29/36 |
| χ2(t)值 | -1.833a | -1.334a | 0.063 | 0.083 | |
| P值 | 0.069 | 0.184 | 0.423 | 0.289 |
| 组别 | 例数 | 基础疾病 | 并发症 | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| NRDS | 新生儿肺炎 | 新生儿败血症 | PDA | 新生儿窒息 | 肺出血 | IVH | 化脓性脑膜炎 | 贫血 | ROP | ||
| 对照组 | 96 | 57(59.4) | 61(63.5) | 68(70.8) | 55(57.3) | 22(22.9) | 3(3.1) | 13(13.5) | 5(5.3) | 72(75.2) | 23(24.0) |
| BPD组 | 65 | 51(78.5) | 62(95.4) | 53(81.5) | 40(61.5) | 38(58.5) | 6(9.2) | 4(6.2) | 6(9.2) | 49(75.4) | 33(50.8) |
| χ2值 | 6.394 | 21.795 | 2.379 | 0.289 | 20.946 | 2.738 | 2.240 | 0.949 | 0.004 | 12.282 | |
| P值 | 0.009 | <0.001 | 0.123 | 0.519 | <0.001 | 0.098 | 0.134 | 0.330 | 0.956 | <0.001 | |
Table 2 Comparison of basic diseases and comorbidities occurrence of preterm infants with and without bronchopulmonary dysplasia
| 组别 | 例数 | 基础疾病 | 并发症 | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| NRDS | 新生儿肺炎 | 新生儿败血症 | PDA | 新生儿窒息 | 肺出血 | IVH | 化脓性脑膜炎 | 贫血 | ROP | ||
| 对照组 | 96 | 57(59.4) | 61(63.5) | 68(70.8) | 55(57.3) | 22(22.9) | 3(3.1) | 13(13.5) | 5(5.3) | 72(75.2) | 23(24.0) |
| BPD组 | 65 | 51(78.5) | 62(95.4) | 53(81.5) | 40(61.5) | 38(58.5) | 6(9.2) | 4(6.2) | 6(9.2) | 49(75.4) | 33(50.8) |
| χ2值 | 6.394 | 21.795 | 2.379 | 0.289 | 20.946 | 2.738 | 2.240 | 0.949 | 0.004 | 12.282 | |
| P值 | 0.009 | <0.001 | 0.123 | 0.519 | <0.001 | 0.098 | 0.134 | 0.330 | 0.956 | <0.001 | |
| 组别 | 例数 | 出生后1 h | 出生后12 h | 出生后24 h | 出生后48 h | 出生后72 h | 出生后96 h | 出生后5 d | 出生后6 d | 出生后7 d |
|---|---|---|---|---|---|---|---|---|---|---|
| 对照组 | 96 | 0.69±0.21 | 1.23±0.27 | 1.41±0.24 | 1.66±0.27 | 1.93±0.32 | 2.21±0.30 | 2.39±0.32 | 2.36±0.32 | 2.38±0.33 |
| BPD组 | 65 | 0.41±0.17 | 0.96±0.20 | 1.22±0.27 | 1.62±0.27 | 1.87±0.31 | 2.24±0.28 | 2.31±0.28 | 2.30±0.26 | 2.31±0.27 |
| t值 | -9.036 | -6.980 | -4.569 | -0.929 | -1.326 | 0.511 | -1.669 | -1.144 | -1.435 | |
| P值 | <0.001 | <0.001 | <0.001 | 0.354 | 0.187 | 0.610 | 0.097 | 0.254 | 0.153 |
Table 3 Comparison of perfusion index values after deliver between preterm infants with and without bronchopulmonary dysplasia at different time periods
| 组别 | 例数 | 出生后1 h | 出生后12 h | 出生后24 h | 出生后48 h | 出生后72 h | 出生后96 h | 出生后5 d | 出生后6 d | 出生后7 d |
|---|---|---|---|---|---|---|---|---|---|---|
| 对照组 | 96 | 0.69±0.21 | 1.23±0.27 | 1.41±0.24 | 1.66±0.27 | 1.93±0.32 | 2.21±0.30 | 2.39±0.32 | 2.36±0.32 | 2.38±0.33 |
| BPD组 | 65 | 0.41±0.17 | 0.96±0.20 | 1.22±0.27 | 1.62±0.27 | 1.87±0.31 | 2.24±0.28 | 2.31±0.28 | 2.30±0.26 | 2.31±0.27 |
| t值 | -9.036 | -6.980 | -4.569 | -0.929 | -1.326 | 0.511 | -1.669 | -1.144 | -1.435 | |
| P值 | <0.001 | <0.001 | <0.001 | 0.354 | 0.187 | 0.610 | 0.097 | 0.254 | 0.153 |
| 组别 | 例数 | 入院后1 h | 入院后12 h | 入院后24 h |
|---|---|---|---|---|
| 对照组 | 96 | 3.15±2.32 | 1.53±0.56 | 1.19±0.43 |
| BPD组 | 65 | 5.02±1.88 | 1.83±0.82 | 1.20±0.39 |
| t值 | 5.377 | 1.464 | 0.134 | |
| P值 | <0.001 | 0.145 | 0.894 |
Table 4 Lactic acid value comparison between preterm infants with and without bronchopulmonary dysplasia at different time periods after admission
| 组别 | 例数 | 入院后1 h | 入院后12 h | 入院后24 h |
|---|---|---|---|---|
| 对照组 | 96 | 3.15±2.32 | 1.53±0.56 | 1.19±0.43 |
| BPD组 | 65 | 5.02±1.88 | 1.83±0.82 | 1.20±0.39 |
| t值 | 5.377 | 1.464 | 0.134 | |
| P值 | <0.001 | 0.145 | 0.894 |
| 组别 | 例数 | 监测1 h | 监测12 h | 监测24 h |
|---|---|---|---|---|
| 对照组 | 17 | 36±2 | 37±3 | 37±2 |
| BPD组 | 16 | 35±4 | 36±3 | 37±3 |
| t值 | -0.806 | -0.870 | 0.584 | |
| P值 | 0.426 | 0.391 | 0.564 |
Table 5 Comparison of mean arterial pressure levels between critical and extremely critical preterm infants with and without bronchopulmonary dysplasia at different time periods
| 组别 | 例数 | 监测1 h | 监测12 h | 监测24 h |
|---|---|---|---|---|
| 对照组 | 17 | 36±2 | 37±3 | 37±2 |
| BPD组 | 16 | 35±4 | 36±3 | 37±3 |
| t值 | -0.806 | -0.870 | 0.584 | |
| P值 | 0.426 | 0.391 | 0.564 |
| [1] | ENDO T, SAMPEI M, FUKUDA S. Kangaroo mother care alters chromogranin A and perfusion index in preterm babies[J]. Pediatr Int,2021,63(1):53-59. DOI:10.1111/ped.14350. |
| [2] | PLANA M N, ZAMORA J, SURESH G,et al. Pulse oximetry screening for critical congenital heart defects[J]. Cochrane Database Syst Rev,2018,3:CD011912. DOI:10.1002/14651858.CD011912.pub2. |
| [3] | 易琳,杨传忠,李欢,等. 灌注指数以及灌注变异指数在早产儿动脉导管未闭中的应用[J]. 中国医学创新,2019,16(13):134-136. DOI:10.3969/j.issn.1674-4985.2019.13.034. |
| [4] | 邵肖梅,叶鸿瑁,丘小汕. 实用新生儿学[M]. 5版. 北京:人民卫生出版社,2019:727-732. 0-347. |
| [5] | 魏克伦,陈克正,孙眉月,等. 新生儿危重病例评分法(草案)[J]. 中华儿科杂志,2001,39(1):42-43. DOI:10.3760/j.issn:0578-1310.2001.01.013. |
| [6] | ECKERT G U, FORTES FILHO J B, MAIA M,et al. A predictive score for retinopathy of prematurity in very low birth weight preterm infants[J]. Eye(Lond),2012,26(3):400-406. DOI:10.1038/eye.2011.334. |
| [7] | STEURER M A, NAWAYTOU H, GUSLITS E,et al. Mortality in infants with bronchopulmonary dysplasia:data from cardiac catheterization[J]. Pediatr Pulmonol,2019,54(6):804-813. DOI:10.1002/ppul.24297. |
| [8] | FINE-GOULDEN M R, DURWARD A. How to use lactate[J]. Arch Dis Child Educ Pract Ed,2014,99(1):17-22. DOI:10.1136/archdischild-2013-304338. |
| [9] | 费菲,王仲.《急性循环衰竭中国急诊临床实践专家共识》解读——病理生理、早期识别与诊断部分[J]. 中国医药科学,2016,6(9):1-5. |
| [10] | LIMA A, BAKKER J. Noninvasive monitoring of peripheral perfusion[J]. Intensive Care Med,2005,31(10):1316-1326. DOI:10.1007/s00134-005-2790-2. |
| [11] | DE FELICE C, DEL VECCHIO A, CRISCUOLO M,et al. Early postnatal changes in the perfusion index in term newborns with subclinical chorioamnionitis[J]. Arch Dis Child Fetal Neonatal Ed,2005,90(5):F411-414. DOI:10.1136/adc.2004.068882. |
| [12] | JEGATHEESAN P, SONG D L, ANGELL C,et al. Oxygen saturation nomogram in newborns screened for critical congenital heart disease[J]. Pediatrics,2013,131(6):e1803-1810. DOI:10.1542/peds.2012-3320. |
| [13] | CHOUDHARY V K, RASTOGI B, SINGH V P,et al. Comparison of hemodynamic responses along with perfusion index to tracheal intubation with Macintosh and McCoy laryngoscopes[J]. Int J Res Med Sci,2018,6(5):1673. DOI:10.18203/2320-6012.ijrms20181757. |
| [14] | KROESE J K, VAN VONDEREN J J, NARAYEN I C,et al. The perfusion index of healthy term infants during transition at birth[J]. Eur J Pediatr,2016,175(4):475-479. DOI:10.1007/s00431-015-2650-1. |
| [15] | ALDERLIESTEN T, LEMMERS P M, BAERTS W,et al. Perfusion index in preterm infants during the first 3 days of life:reference values and relation with clinical variables[J]. Neonatology,2015,107(4):258-265. DOI:10.1159/000370192. |
| [16] | CORSINI I, CECCHI A, COVIELLO C,et al. Perfusion index and left ventricular output correlation in healthy term infants[J]. Eur J Pediatr,2017,176(8):1013-1018. DOI:10.1007/s00431-017-2920-1. |
| [17] | TUTEN A, DINCER E, TOPCUOGLU S,et al. Serum lactate levels and perfusion index:are these prognostic factors on mortality and morbidity in very low-birth weight infants?[J]. J Matern Fetal Neonatal Med,2017,30(9):1092-1095. DOI:10.1080/14767058.2016.1205019. |
| [18] | 章斌,雷小平,康兰,等. 无创心输出量测量仪在早产儿支气管肺发育不良早期预测中的价值研究[J]. 重庆医学,2020,49(23):3884-3888. DOI:10.3969/j.issn.1671-8348.2020.23.005. |
| [19] | ALLEN M. Lactate and acid base as a hemodynamic monitor and markers of cellular perfusion[J]. Pediatr Crit Care Med,2011,12(4 ):S43-49. DOI:10.1097/PCC.0b013e3182211aed. |
| [20] | HATHERILL M, WAGGIE Z, PURVES L,et al. Mortality and the nature of metabolic acidosis in children with shock[J]. Intensive Care Med,2003,29(2):286-291. DOI:10.1007/s00134-002-1585-y. |
| [21] | PORYO M, WISSING A, ZEMLIN M,et al. Nucleated red blood cells and serum lactate values on days 2 and 5 are associated with mortality and morbidity in VLBW infants[J]. Wien Med Wochenschr,2019,169(3/4):87-92. DOI:10.1007/s10354-018-0649-8. |
| [22] | HARIRI G, JOFFRE J, LEBLANC G,et al. Narrative review:clinical assessment of peripheral tissue perfusion in septic shock[J]. Ann Intensive Care,2019,9(1):37. DOI:10.1186/s13613-019-0511-1. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||